Laser Treatment Scar Revision and Other Ways to Surgery Scars
Surgery scars can be meaningfully improved with the right intervention. Discover what clinical evidence says about laser revision, topical therapies, and other treatments for post-surgical scars.

What Clinical Evidence Says About Surgery Scar Treatment
Surgery scar treatment encompasses a range of interventions — from simple topical products to surgical revision — that can meaningfully reduce a scar's size, color, texture, and discomfort, even if no treatment can eliminate a scar completely.
Quick reference: evidence-based surgery scar treatment options
| Treatment | Best for | When to start |
|---|---|---|
| Silicone gel sheets or gel | Hypertrophic, raised scars | Once wound is fully closed |
| Sun protection (SPF 30+) | All scar types | From ~3 weeks post-surgery |
| Scar massage | Firm, tight scars | Around 3 weeks post-surgery |
| Steroid injections | Raised, keloid, or hypertrophic scars | After scar matures |
| Laser therapy | Discolored, textured, or raised scars | As directed by a clinician |
| Surgical revision (Z-plasty, grafting) | Contractures, severe scarring | After 12-18 months |
Scarring is a normal part of how skin repairs itself after surgery. The body lays down new collagen fibers to close the wound — but that new tissue rarely looks or behaves exactly like the original skin.
What many people don't realize is that a scar is not finished forming at the moment the wound closes. Research consistently shows that surgical scars continue to remodel for up to 12 to 18 months after the procedure. A scar that looks red and raised at three months may flatten and fade considerably by the one-year mark.
That timeline matters enormously when choosing a treatment strategy. Acting too early — or waiting too long — can affect outcomes. And because scar formation is influenced by genetics, skin tone, wound location, surgical technique, and aftercare, no single treatment works for every scar or every person.
This guide reviews what the clinical evidence actually shows about the most widely used surgery scar treatments, from non-invasive first-line options to advanced medical procedures.
The Biological Mechanism of Post-Surgical Wound Healing
Understanding surgery scar treatment begins with the biological phases of repair. When the skin is incised, the body initiates a complex four-stage cascade: hemostasis (clotting), inflammation, proliferation (building new tissue), and remodeling.
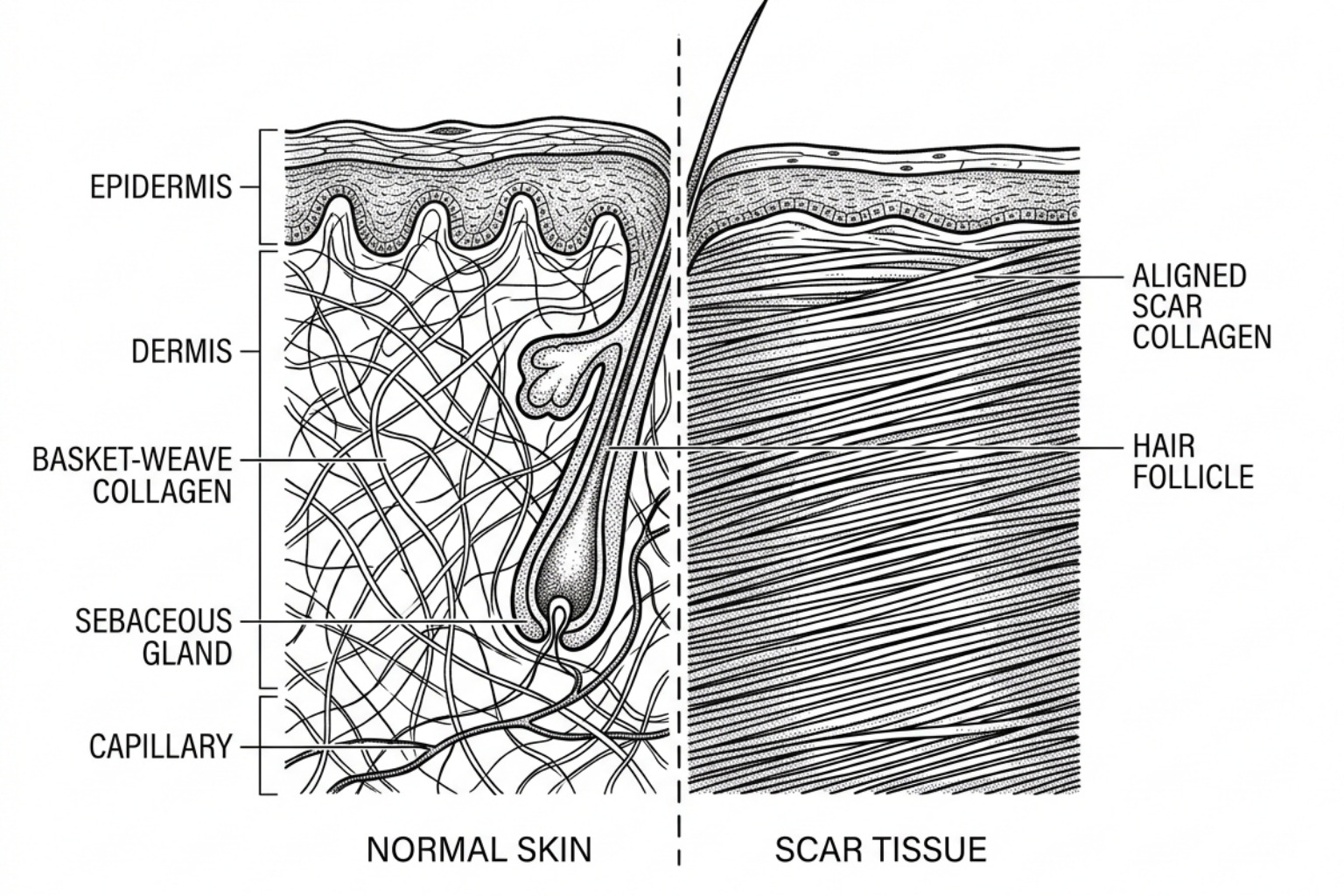
During the proliferative phase, cells called fibroblasts migrate to the wound site to produce collagen, the structural protein of the skin. In healthy, unscarred tissue, collagen fibers are woven in a complex, basket-weave pattern. In a scar, however, these fibers align in a single direction, which results in a different texture and less flexibility.
Clinical data indicates that at six weeks post-injury, the wound has regained only about 50% of the skin's original tensile strength. By three months, this reaches approximately 80%, which is the maximum strength a scar can achieve. The final phase, remodeling, is a long-term process. Over 12 to 18 months, the body continuously breaks down and replaces collagen. This is why medical professionals often suggest waiting at least a year before pursuing invasive surgical scar revision because the tissue is still naturally evolving.
Clinical Classification of Surgical Scars
Not all surgical scars are identical. Their classification determines the most appropriate clinical approach.
- Hypertrophic Scars: These are raised and red but remain within the boundaries of the original surgical incision. They often develop within weeks of surgery and may partially regress on their own over a year.
- Keloids: These are thick, irregular clusters of scar tissue that grow beyond the edges of the original wound. They are caused by overactive fibroblasts and can appear up to a year after the initial trauma. Research shows they are more common in individuals with darker skin tones or red hair.
- Contractures: Often resulting from large areas of skin loss or incisions that cross joints, these scars pull the edges of the skin together, potentially restricting muscle or joint movement.
- Atrophic Scars: These appear as sunken recesses in the skin, often occurring when the underlying structure (like fat or muscle) is lost or when collagen production is insufficient during healing.
Comparison of Pathological Scar Characteristics
| Feature | Hypertrophic Scar | Keloid Scar |
|---|---|---|
| Growth Pattern | Stays within wound margins | Extends beyond wound margins |
| Onset | Usually within 4 weeks | Can be delayed (up to 1 year) |
| Natural Regression | May flatten over time | Rarely regresses spontaneously |
| Recurrence Risk | Low after simple excision | High (up to 100% without adjunct therapy) |
The Cleveland Clinic notes that the goal of revision is rarely total erasure, but rather matching the surrounding skin's color and texture.
Evidence-Based Surgery Scar Treatment: Topical and Non-Invasive Interventions
For many patients, the first line of defense involves non-invasive topical agents. Clinical consensus identifies silicone-based products as the gold standard for at-home management.
Silicone Gel and Sheets Silicone works by creating an occlusive barrier that mimics the skin's stratum corneum. This increases hydration in the scar tissue, which signals the fibroblasts to scale back collagen production. Research suggests that for maximum efficacy, silicone sheets should be worn for 12 to 24 hours a day for several months. For visible areas like the face, silicone gels offer a more discreet alternative.
Pressure Therapy Often used for hypertrophic and keloid scars, pressure garments or bandages apply mechanical force to the tissue. This reduces blood flow to the area, limiting the oxygen and nutrients available to the overactive fibroblasts. This method is common in abdomen scar reduction and burn recovery.
Hydration and Moisture Retention Keeping the wound moist is critical during the early stages. Evidence suggests that a moist environment accelerates re-epithelialization (the growth of new skin cells) more effectively than letting a hard scab form. Using simple petrolatum (petroleum jelly) can prevent the wound from drying out and reduce the likelihood of a thick scar forming. This is a foundational step in non-invasive C-section care.
Non-Invasive Surgery Scar Treatment and Prevention
The most effective surgery scar treatment is often preventative.
- Sun Protection: New scar tissue is highly sensitive to ultraviolet (UV) radiation. Exposure to the sun can cause permanent hyperpigmentation, making the scar darker and more noticeable. Clinical guidelines recommend using broad-spectrum SPF 30+ or keeping the scar covered for at least 12 to 18 months.
- Early Wound Care: Following post-surgery care instructions—such as keeping the area clean and avoiding tension on the incision—is vital. Avoiding habits like smoking is also essential, as nicotine restricts blood flow and significantly impairs the healing process.
- Tension Reduction: Surgeons use specific techniques to ensure wound edges are everted (turned slightly outward) during closure, which helps the scar lay flat once it heals.

Advanced Clinical Modalities for Surgery Scar Treatment
When topical treatments are insufficient, clinical procedures can offer more significant remodeling.
Laser Resurfacing Lasers are used to target different aspects of a scar.
- V-Beam (Pulsed Dye Laser): Uses a 595 nm wavelength to target blood vessels, effectively reducing the redness of a fresh or hypertrophic scar.
- Fractional CO2 Laser: Creates microscopic columns of injury in the skin to trigger a new, more organized healing response. This is often used for laser treatment for surgical scars to improve texture and flexibility. You can view clinical outcomes in CO2 laser results documentation.
Injections
- Corticosteroids: These are the first-line treatment for keloids and hypertrophic scars. Injected directly into the tissue, they break down collagen bonds and reduce inflammation, helping the scar to flatten and soften.
- 5-Fluorouracil (5-FU): A chemotherapy agent that, when injected in small doses, can inhibit fibroblast proliferation in stubborn keloids.
Cryotherapy This involves freezing the scar tissue from the inside out using liquid nitrogen. It is often combined with steroid injections to improve the penetration of the medication.
Surgical Approaches to Surgery Scar Treatment
In cases where a scar is functionally restrictive or aesthetically distressing, a secondary surgery may be required. This is known as surgical scar revision.
- Z-Plasty: A technique where the surgeon creates triangular flaps to reorient the scar. This can help the scar follow natural skin folds and release tension that causes contractures.
- Skin Grafting: Used for large scars, such as those from burns, where healthy skin is moved from a donor site to the scarred area.
- Tissue Expansion: A silicone balloon is inserted under healthy skin near the scar and gradually filled with saline over several weeks. This stretches the healthy skin, which is then used to replace the scarred tissue once it is excised.
The American Society of Plastic Surgeons emphasizes that while these techniques improve appearance, they still involve creating a new incision, which requires its own diligent aftercare.
Frequently Asked Questions about Surgery Scar Treatment
When should scar massage be initiated?
Scar massage is a mechanical method used to break up excess collagen and increase the flexibility of the tissue. Clinical consensus suggests starting scar tissue massage therapy approximately three weeks after surgery, provided the wound is completely closed and any scabs have fallen off.
The general technique involves using a lubricant (like aqueous cream) and applying firm, circular pressure over the scar for 5 to 10 minutes, two to three times daily. This mechanical tension helps realign collagen fibers and can reduce the "hardness" often felt in maturing scars.
What are the primary risks of scar revision procedures?
While revision aims to improve the skin, it is not without risks. Potential complications include:
- Infection or Bleeding: Common risks with any surgical procedure.
- Keloid Recurrence: Keloids have a high rate of returning, sometimes larger than before, if surgery is not paired with radiation or injections.
- Hyperpigmentation: The new incision may darken if not protected from the sun.
- Wound Dehiscence: The edges of the new wound may pull apart if there is too much tension or premature activity.
When is a medical consultation necessary for a scar?
While most scars are a cosmetic concern, you should seek professional advice if:
- The scar is painful, persistently itchy, or shows signs of infection (pus, warmth, extreme swelling).
- The scar restricts your range of motion or "pulls" at a joint.
- A keloid is rapidly expanding beyond the original wound borders.
- The appearance of the scar is causing significant psychological distress or impacting your quality of life.
Conclusion
Managing a surgical scar is a marathon, not a sprint. From the initial inflammatory response to the final remodeling phase 18 months later, the body is in a constant state of flux. By utilizing a multimodal approach—combining early moisture retention, consistent sun protection, and advanced clinical interventions like lasers or injections—it is possible to significantly improve the final outcome.
If you are concerned about the progression of your healing, you can start your professional scar assessment to better understand your options and set realistic expectations for your skin's recovery.
Works Cited
- American Society of Plastic Surgeons. "Scar Revision."
- Cleveland Clinic. "Scar Revision: What It Is, Who Is a Candidate and Treatment Options."
- MedlinePlus Medical Encyclopedia. "Scar revision."
- NHS. "Scars - Treatment."
- Journal of Clinical and Aesthetic Dermatology. "Update on Postsurgical Scar Management."
This content is for informational purposes only and does not constitute medical advice. Consult a qualified healthcare professional for diagnosis and treatment.