Best Surgical Scar Concealer for Sensitive Skin

Clinical Considerations for Surgical Scar Concealment on Sensitive Skin
Effective options for a surgical scar concealer on sensitive skin typically share several key clinical properties:
- Non-comedogenic and hypoallergenic — formulated to avoid occluding pores or triggering allergic responses in healing tissue.
- Fragrance-free and alcohol-free — minimizes the risk of contact dermatitis and barrier disruption.
- High pigment density — allows for coverage of dyschromia and texture irregularities with minimal product layers.
- Waterproof and transfer-resistant — ensures durability for post-operative patients.
- Available in two primary formats: topical silicone fillers (for recessed scars) and high-coverage pigmented creams (for surface discoloration).
Surgical scars result from the physiological wound-healing process. Following an incision, the synthesis of new collagen fibers repairs the tissue, though the resulting architecture often differs from the surrounding dermis in color, texture, and elevation. For many individuals, visible scarring on exposed areas can impact psychological well-being during the remodeling phase.
Standard cosmetic foundations are generally formulated for healthy, intact skin and often lack the pigment concentration or adhesive properties required to mask significant texture irregularities or deep discoloration. Medical-grade camouflage products are designed to address these specific needs. For those with sensitive skin, the primary objective is achieving adequate coverage without inducing irritation or interfering with the underlying biological healing process.
Pathophysiology of Surgical Scars and the Role of Camouflage
To understand the function of a surgical scar concealer, it is necessary to examine the biological repair mechanism. When an incision occurs, the inflammatory response triggers fibroblasts to produce collagen. Unlike the organized, "basket-weave" structure of healthy dermis, scar collagen is often deposited in dense, parallel bundles.
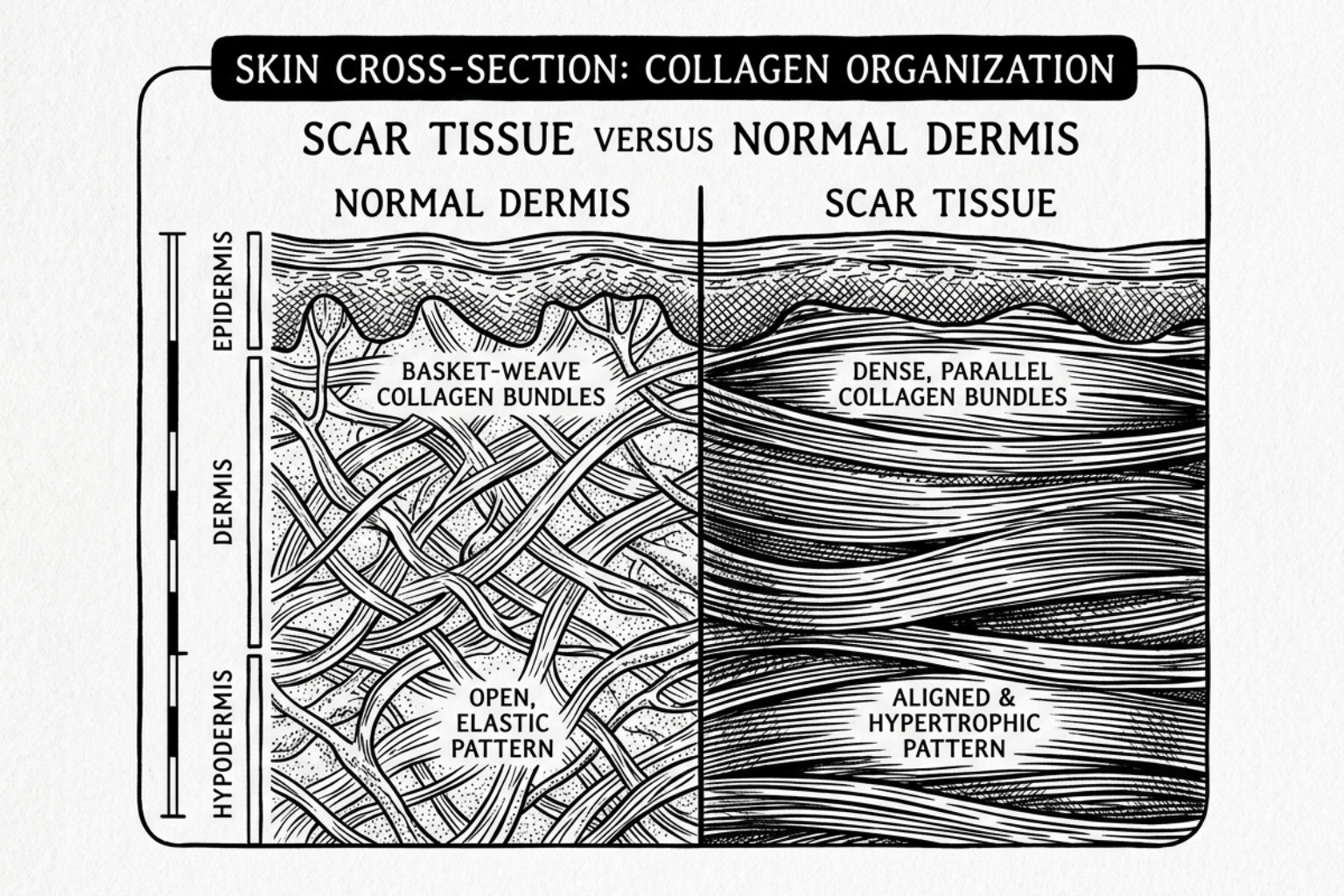
This structural variance leads to different scar morphologies:
- Hypertrophic Scars: Raised, erythematous lesions that remain within the original wound boundaries, often flattening over 12 to 24 months.
- Keloids: Excessive scar tissue extending beyond the initial incision site; research suggests genetic predispositions may influence their formation.
- Atrophic Scars: Depressed areas resulting from tissue loss, frequently observed after procedures such as Mohs surgery.
Medical camouflage acts as a corrective layer that mimics the optical properties of healthy skin. While Post-Surgery Scar Care focuses on biological remodeling, concealment utilizes light refraction and pigment correction to minimize the visual prominence of the scar.
Distinguishing Medical Camouflage from Traditional Cosmetics
Traditional cosmetics typically contain 15% to 20% pigment. In contrast, a specialized surgical scar concealer or medical camouflage cream often contains 40% to 50% pigment. This density allows for effective coverage with a single application, reducing the mechanical friction required during use—a critical factor for sensitive skin.
Furthermore, many medical-grade products are anhydrous or silicone-based. Unlike traditional makeup that may use comedogenic waxes, silicone-based concealers create a flexible, breathable film with a refractive index similar to human skin, preventing an artificial appearance.
Clinical Requirements for Surgical Scar Concealment
When evaluating a surgical scar concealer, clinical efficacy is determined by its ability to protect the skin barrier while providing aesthetic correction. A primary concern in scar management is Transepidermal Water Loss (TEWL). Scars often lack a fully functional barrier, leading to dehydration that can exacerbate the scar's appearance.
Evidence suggests that topical silicone is a primary non-invasive intervention for scar management. It creates an occlusive environment that hydrates the stratum corneum, which may help regulate fibroblast activity. Therefore, a concealer incorporating silicone provides both cosmetic coverage and a protective environment. For long-term improvement, utilizing the Best Scar Reduction Cream alongside camouflage is often recommended by dermatologists.
Selection Criteria for Surgical Scar Concealer in Sensitive Skin Patients
Post-operative skin is frequently reactive. The clinical goal is to avoid contact dermatitis. Research indicates that several common additives should be avoided:
- Fragrance: Synthetic scents are a leading cause of cosmetic-related skin reactions.
- Parabens: While used as preservatives, some patients may experience irritation on healing tissue.
- Alcohol: Denatured alcohol can dehydrate the skin and compromise the fragile healing barrier.
Hypoallergenic testing is a standard benchmark where products are tested to ensure a low incidence of allergic reactions. For surgical patients, this is a critical safety feature.
Performance Analysis of Medical Camouflage Options
Beyond safety, a surgical scar concealer must meet specific performance criteria:
- Smudge-proof and Transfer-resistant: The product should remain stable against clothing or dressings.
- Durability: Many patients require coverage that lasts through daily activities without reapplication.
- Matte Finish: Scars often appear "shiny" due to the absence of sweat glands; a matte finish helps neutralize this sheen.
- UV Protection: UV exposure can cause permanent hyperpigmentation in healing scars. Many medical concealers include mineral filters like titanium dioxide.
Comparative Analysis of Topical Fillers and Pigmented Creams
The selection of a surgical scar concealer depends on the topography of the tissue.
| Feature | Topical Silicone Fillers | High-Pigment Camouflage Creams |
|---|---|---|
| Primary Use | Recessed/Atrophic scars | Discoloration/Redness (flat scars) |
| Texture | Clear or tinted gel | Thick, opaque cream |
| Mechanism | Fills depressions to level skin | Masks color with pigment |
| Longevity | Waterproof; 12-24 hours | Water-resistant; requires setting |
| Best For | Acne scars, Mohs surgery sites | Incisions, bruising, flat scars |
Mechanism of Topical Silicone Fillers
For recessed surgical scars, traditional creams may fail because they do not address the shadow created by the depression. Topical silicone fillers utilize cross-linked polymers to address this. These products are applied as a gel and dry into a flexible, skin-mimetic film. By physically filling the indentation, they can significantly reduce the visibility of deep scars, providing an alternative for those considering Surgical Scar Revision.
Efficacy of High-Coverage Camouflage Creams
For flat scars with significant erythema or bruising, high-coverage creams are the clinical standard. These products utilize mineral pigments, such as iron oxides, to provide total opacity. Because these creams often have a high pigment load, they typically require a setting powder to ensure they become smudge-proof. The powder creates a bond with the cream, securing it for extended wear.
Evidence-Based Application Protocols for Post-Operative Tissue
Application technique is just as important as the product itself. Applying makeup to a surgical site requires a "low-friction" approach to avoid disrupting the tissue.
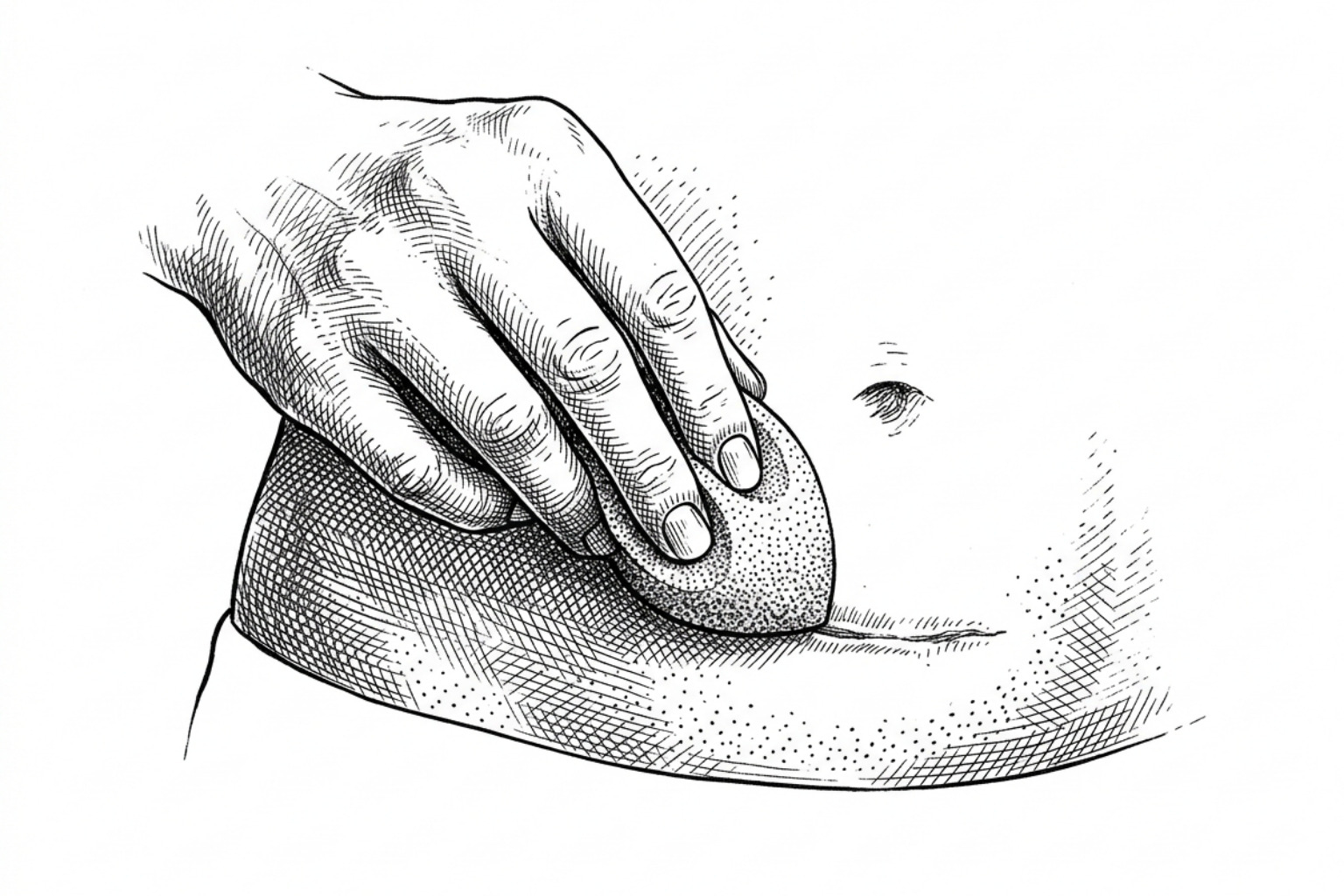
- Preparation: Ensure the wound is fully closed (no scabs or open areas). Cleanse with a mild, oil-free cleanser.
- Color Correction: If the scar is very red, a thin layer of green-tinted corrector can neutralize the hue. For scars that appear blue or purple (common in bruising), a peach or orange corrector is more effective.
- Stippling: Instead of rubbing, use a "stippling" or tapping motion with a damp sponge or clean fingertip. This deposits pigment without pulling on the skin.
- Setting: Apply a translucent setting powder using a "press and roll" motion with a powder puff.
For those dealing with persistent redness or thickening, combining camouflage with Laser Treatment for Surgical Scars can address the underlying vascularity while the makeup provides immediate relief.
Optimization of Surgical Scar Concealer Longevity and Stability
To make a surgical scar concealer last all day, avoid using heavy oil-based moisturizers immediately before application, as these can break down the pigments. Instead, use a silicone-based primer or a lightweight, oil-free lotion. For removal, use a gentle, water-based makeup remover or micellar water to dissolve the product without aggressive scrubbing.
Clinical Inquiries Regarding Surgical Scar Camouflage
Temporal Guidelines for Post-Operative Application
Clinical consensus suggests waiting until the wound is completely closed and any sutures or staples have been removed. This usually occurs between 10 to 14 days post-surgery. Applying makeup to an open wound or a scabbed area increases the risk of infection and can trap bacteria, potentially leading to a worse scar. Always consult your surgeon before the first application.
Impact of Medical Camouflage on Biological Wound Healing
When using high-quality, non-comedogenic, and breathable products (like those based on silicone), camouflage should not interfere with healing. In fact, silicone-based products may support the healing environment by maintaining hydration. However, using "drugstore" makeup that contains heavy oils, fragrances, or comedogenic ingredients can cause inflammation or breakouts around the scar site.
Efficacy of Topical Fillers in Hypertrophic and Keloid Scarring
Topical fillers are designed to level the skin by filling in "holes" or depressions. They are highly effective for atrophic (recessed) scars. For raised keloids or hypertrophic scars, fillers are less effective at changing the silhouette. In these cases, a high-pigment cream is better suited to neutralize the redness and help the raised area blend into the surrounding skin tone.
Conclusion
The process of recovery involves both physiological and psychological components. A surgical scar concealer serves as a tool for restoring confidence during the long remodeling phase of a scar. When selecting a product, priority should be given to medical-grade formulations that are hypoallergenic and fragrance-free, particularly for sensitive skin.
Whether utilizing a topical silicone filler for depth or a high-coverage cream for color, the objective is to provide a protective, breathable barrier that allows for social comfort while the tissue heals. For those uncertain of their scar type, performing a Scar Assessment can help determine if a scar is hypertrophic, keloid, or atrophic, which guides the choice of both concealment and treatment.
Works Cited
- Monstrey, S., et al. (2014). "Updated scar management practical guidelines: non-invasive and invasive measures." Journal of Plastic, Reconstructive & Aesthetic Surgery.
- Gold, M. H., et al. (2014). "International clinical recommendations on scar management." Dermatologic Surgery.
- O'Connell, J. T., et al. (2012). "The use of medical camouflage in dermatology." Journal of Clinical and Aesthetic Dermatology.
Disclaimer: This content is for informational purposes only and does not constitute medical advice. Consult a qualified healthcare professional for diagnosis and treatment.