How to Treat Burn Scars Without Surgery
Burn scars can be effectively managed without surgery. Explore evidence-based non-invasive therapies including silicone sheets, pressure garments, and topical treatments for burn scar recovery.
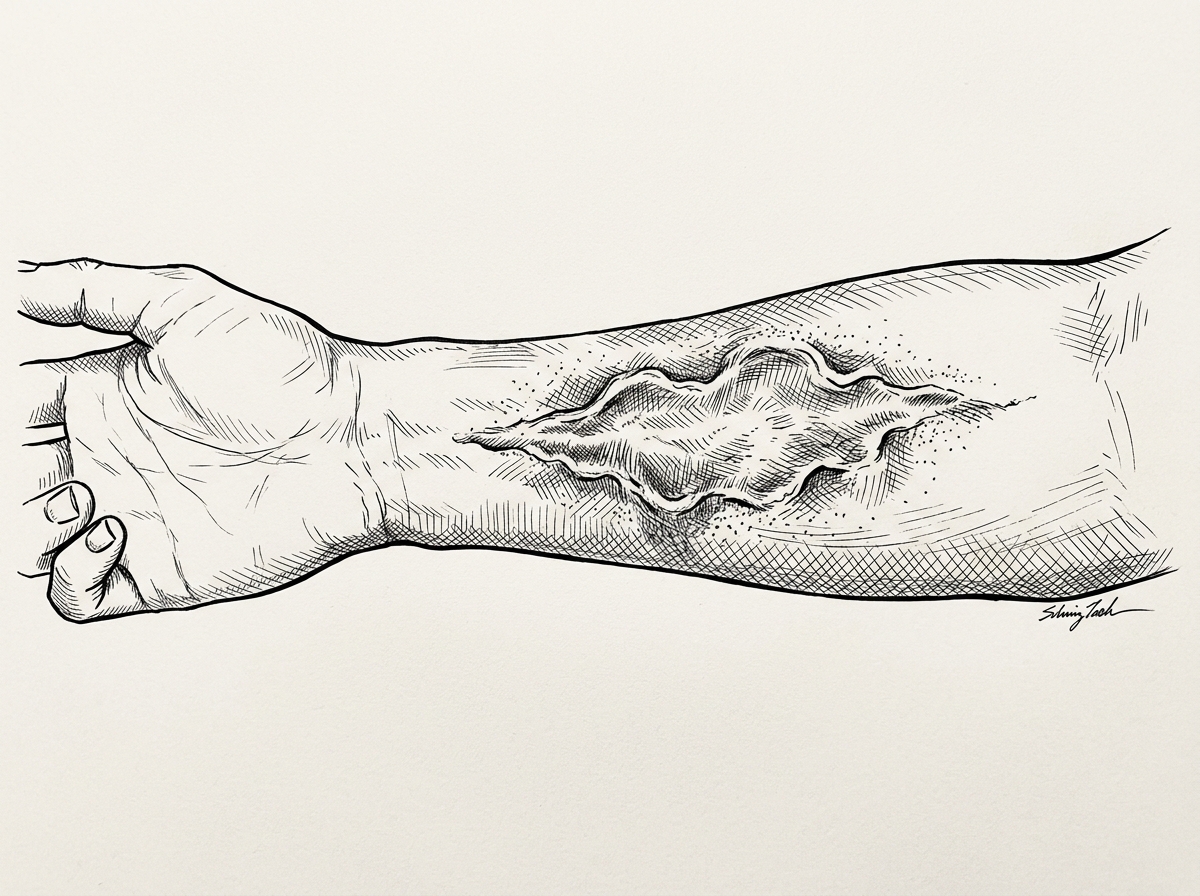
Non-Surgical Treatment for Burn Scars: What the Evidence Shows
Non surgical burn scars can be managed effectively without an operating room. For most people, a combination of evidence-based, non-invasive therapies is the first — and often most appropriate — line of treatment.
Quick answer: the main non-surgical options for burn scars include:
| Treatment | Primary Benefit | Typical Duration |
|---|---|---|
| Compression therapy | Reduces scar height and erythema | 8-24 months, 23 hrs/day |
| Silicone gel sheets | Hydrates and flattens raised scars | 12-16 hrs/day for 3-6 months |
| Massage therapy | Improves pliability and VSS score | Ongoing during maturation phase |
| Pulsed dye laser (PDL) | Reduces redness and inflammation | 3-6 sessions, starting ~3 months post-healing |
| Fractional CO2 laser | Reduces scar thickness | 3-6 sessions |
| Microneedling | Improves texture and joint mobility | Multiple sessions |
| Sun protection (SPF 30+) | Prevents discoloration | Ongoing |
Burn injuries are more common than many people realize. According to the World Health Organization, nearly 11 million people worldwide sustain burns severe enough to need medical attention every year. In the United States alone, roughly half a million people suffer serious burns annually.
The aftermath of a burn injury often extends well beyond the initial wound. Between 30% and 90% of burn survivors go on to develop pathological scarring — tissue that is thickened, raised, tight, or discolored compared to surrounding skin. More than one million people in the U.S. seek treatment for problematic scars each year.
Scars are a natural part of healing — but that does not mean patients have to accept significant functional or cosmetic impairment without intervention. Burn scar tissue continues to remodel for anywhere from 8 months to 2 years after injury. That extended maturation window is also an opportunity: the right non-surgical strategies, applied consistently and at the right time, can meaningfully change how a scar develops.
The evidence base for non-surgical approaches has grown considerably over the past decade. A 2025 network meta-analysis published in PLOS One — drawing on 17 randomized controlled trials across 11 countries — found that massage therapy ranked highest for improving overall scar quality, while fractional CO2 laser therapy ranked highest for reducing scar thickness. These are not experimental ideas; they are clinically studied interventions with measurable outcomes.
This guide explains the biology behind burn scar formation, reviews the clinical evidence for each major non-surgical treatment, and outlines realistic expectations for recovery.
Pathophysiology of Burn Scar Formation and Tissue Remodeling
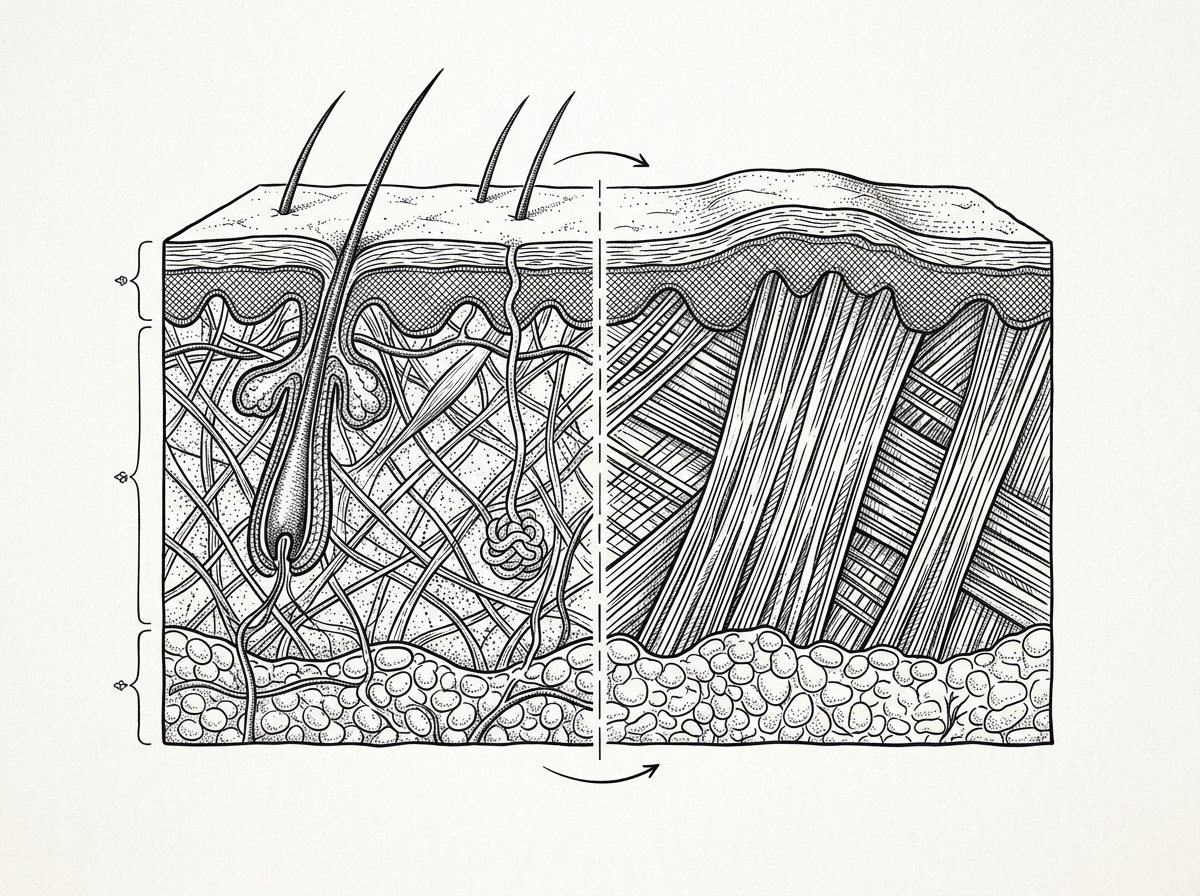
Understanding how non surgical burn scars respond to treatment requires a look at the cellular level. When the dermis (the deep layer of skin) is damaged by heat, the body initiates a complex repair sequence. This process is driven primarily by fibroblasts, the "construction workers" of the skin.
In normal wound healing, fibroblasts produce collagen to bridge the gap in the tissue. However, in deep burns, the inflammatory response is often prolonged. This leads to an overproduction of collagen and an architectural mess in the extracellular matrix. Instead of the organized, basket-weave pattern found in healthy skin, scar collagen is often laid down in thick, parallel bundles.
According to the ISBI Practice Guidelines for Burn Care, the risk of pathological scarring increases significantly if a wound takes longer than 14 to 21 days to heal. During this window, the body’s healing aptitude shifts into high gear, unleashing inflammatory cells and blood vessels. If this process isn't modulated, the result is a scar that lacks the hair follicles, sweat glands, and elastic fibers of normal skin, often appearing shiny or rigid.
Clinical Classification of Non Surgical Burn Scars
Medical professionals use specific categories to describe how burn scars behave and appear. Identifying the type of scar is the first step in choosing the correct non-surgical path. A 2025 network meta-analysis on non-surgical treatments emphasizes that different modalities target specific clinical features, such as thickness or pliability.
The Vancouver Scar Scale (VSS) is the gold-standard tool used by clinicians to assess these scars. It scores four variables:
- Vascularity: The amount of redness (erythema).
- Pliability: How flexible or stiff the tissue is.
- Pigmentation: How the color compares to the surrounding skin.
- Height: The thickness or elevation of the scar.
Identifying Hypertrophic Non Surgical Burn Scars
Hypertrophic scars are the most common complication of burn injuries. These scars are raised, red, and firm, but they stay within the boundaries of the original injury. They typically appear 2 to 6 weeks after the skin has closed and continue to grow for 6 to 12 months. Symptoms often include intense itching (pruritus), pain, and a feeling of tightness that can restrict movement, especially if the scar is located over a joint like the elbow or chest.
Distinguishing Keloids from Hypertrophic Tissue
While similar in appearance, keloids are more aggressive. Unlike hypertrophic scars, keloids invade healthy surrounding tissue, growing beyond the original burn site. They have a rubbery texture and rarely regress on their own. Genetic factors play a significant role here; individuals with darker skin tones are statistically more likely to develop keloid overgrowth.
Evidence-Based Non-Surgical Interventions for Burn Scars
The goal of non-surgical management is to guide the remodeling process so the scar becomes flatter, softer, and more comfortable.
Compression Therapy
Pressure therapy has been a staple of burn rehabilitation since the late 1960s. By applying constant pressure (ideally between 15 and 30 mmHg), these garments reduce blood flow to the scar and increase the breakdown of excess collagen.
- Protocol: Garments must be worn 23 hours a day, 7 days a week.
- Duration: Treatment continues until the scar matures, which can take 8 to 24 months.
- Maintenance: Garments lose elasticity and should be replaced every 3 months.
Silicone Gel Sheets
Silicone is considered a "gold standard" for preventing and treating hypertrophic scars. Research suggests its primary mechanism is hydration. By occluding the skin, silicone reduces water loss, which signals the fibroblasts to slow down collagen production. For more intensive intervention, some patients utilize microneedling for scar reduction to improve the absorption of topical treatments.
| Feature | Compression Garments | Silicone Gel Sheets |
|---|---|---|
| Mechanism | Mechanical pressure; tissue hypoxia | Hydration and occlusion |
| Best For | Large areas; limbs; torso | Smaller scars; face; joints |
| Wear Time | 23 hours/day | 12-24 hours/day |
| Evidence Level | High (Gold Standard) | High (Gold Standard) |
Laser Therapy Protocols for Non Surgical Burn Scars
Laser technology has transformed burn care by offering "prehabilitation"—improving tissue quality before any necessary surgery, or even replacing the need for surgery entirely. Clinical studies on laser resurfacing show significant improvements in both function and appearance.
- Pulsed Dye Laser (PDL): This laser targets the red color in scars by cauterizing small blood vessels. This reduces inflammation and helps the scar fade faster.
- Fractional CO2 Laser: This laser creates thousands of microscopic holes in the thick scar tissue. This "drilling" effect breaks up stiff collagen bundles and stimulates the growth of more flexible, normal-feeling skin.
The Role of Massage and Physical Rehabilitation
Scar massage is a low-cost, high-impact intervention. A systematic review found that massage therapy is the most effective non-surgical method for improving the overall VSS score, particularly pliability.
Patients are encouraged to use firm, circular friction to help "break up" adhesions between the scar and the underlying muscle or bone. This is especially vital for preventing contractures—where the scar becomes so tight it pulls a joint into a fixed position. For detailed techniques, refer to this guide on scar tissue massage therapy.
Advanced Regenerative Modalities: Lasers and Microneedling
Beyond standard lasers, regenerative medicine is pushing the boundaries of what is possible for non surgical burn scars.
Ablative fractional resurfacing doesn't just "sand down" the scar; it triggers a regenerative immune response. Some centers now use "laser-assisted drug delivery," where the micro-channels created by the CO2 laser are used to deliver anti-inflammatory medications like triamcinolone deep into the dermis.
Microneedling, or percutaneous collagen induction, is another powerful tool. By using a dermaroller for scars, clinicians can create controlled micro-injuries that stimulate a more organized healing response. A study of 15 patients with post-burn hypertrophic scars showed that microneedling significantly improved VSS scores from 8.8 to 4.1, with the best results seen in "acute" scars (those less than one year old).
Long-Term Management and Home Care Strategies
Consistency is the most important factor in non-surgical recovery. Most of the work happens at home, day by day.
- Moisturization: Burned skin lacks natural oils. Applying a water-based, neutral moisturizer at least three times daily helps maintain the skin barrier. For very thick tissue, a hard scar softening massage during lotion application can improve results.
- Sun Protection: New scar tissue is highly sensitive to UV rays. Sun exposure can cause permanent dark staining (hyperpigmentation). Patients should use broad-spectrum SPF 30+ and wear protective clothing for at least one year.
- Wound Care: To minimize a scar from the start, keep the wound moist with petroleum jelly. This prevents scabs from forming; wounds that scab take longer to heal and are more likely to scar deeply.
Frequently Asked Questions about Non-Surgical Burn Recovery
How long does it take for a burn scar to mature?
A burn scar typically takes between 8 months and 2 years to fully mature. During this time, it will transition from being red, hard, and itchy to being softer, flatter, and closer to your natural skin tone.
Is laser therapy for burn scars covered by insurance?
In many cases, yes. While often viewed as cosmetic, insurance companies are increasingly covering laser treatments when they are used to improve "functional" issues, such as reducing chronic pain, intense itching, or restricted joint movement. Documentation from a burn specialist is usually required.
Can massage therapy reduce scar thickness?
While massage is best known for improving pliability (flexibility), it can also help reduce thickness over time by assisting in the remodeling of collagen fibers and reducing edema (swelling) within the scar tissue.
Conclusion
The journey of recovering from a burn injury is often a marathon, not a sprint. However, the data is clear: non surgical burn scars respond remarkably well to consistent, evidence-based care. From the mechanical pressure of compression garments to the regenerative power of fractional lasers, survivors have more options than ever to regain comfort and mobility.
By starting treatments early—often within the first three months of healing—and adhering to a strict regimen of massage, hydration, and protection, patients can significantly influence the final appearance and feel of their skin. For those looking to stay updated on the latest clinical findings in skin regeneration, consider following our non-surgical scar recovery updates.
Works Cited
- Hultman, C. S., et al. (2014). "Laser resurfacing and remodeling of hypertrophic burn scars: The results of a large, prospective, before-after cohort study, with long-term follow-up." Annals of Surgery, 260(3), 519–529.
- ISBI Practice Guidelines for Burn Care. (2016). Burns, 42(5), 953-1021. https://doi.org/10.1016/j.burns.2016.05.013
- Yang, et al. (2025). "Non-surgical treatments for post-burn scars: A network meta-analysis." PLOS One. https://doi.org/10.1371/journal.pone.0330428.g001
- Monstrey, S., et al. (2014). "Updated scar management practical guidelines: non-invasive and invasive measures." Journal of Plastic, Reconstructive & Aesthetic Surgery, 67(8), 1017-1025.
This content is for informational purposes only and does not constitute medical advice. Consult a qualified healthcare professional for diagnosis and treatment.