Scar Assessment & Treatment Evidence Guide
Identify your scar type and explore treatment options ranked by the strength of clinical evidence behind them. Built from peer-reviewed dermatology research.
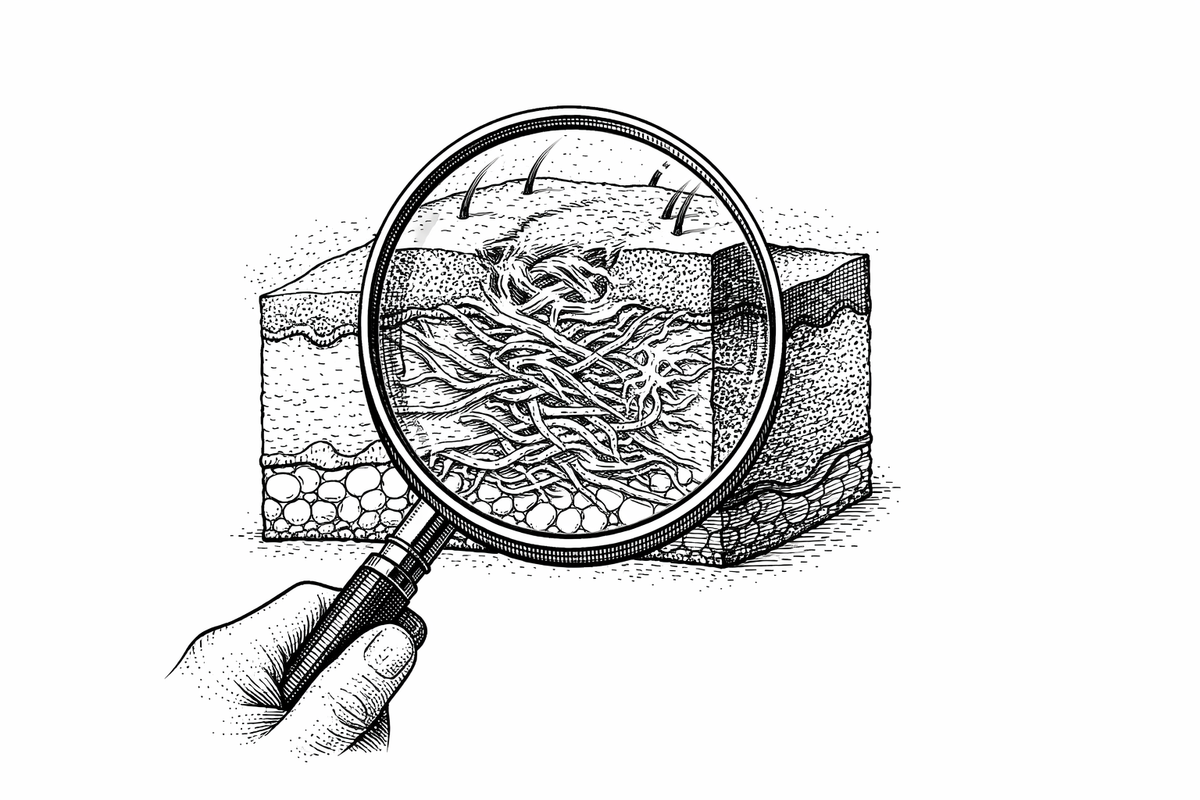
Scar type assessment
Step 1 of 4Your scar type
Treatment evidence for your scar type
Treatments ranked by the strength of published clinical evidence. Evidence levels reflect the quality and quantity of peer-reviewed human studies, not commercial popularity.
| Treatment | Evidence level | Summary of findings |
|---|
Methodology
Evidence levels are assigned based on the following criteria: Strong indicates multiple randomised controlled trials or systematic reviews with consistent findings. Moderate indicates at least one RCT or multiple controlled studies with generally positive outcomes. Limited indicates small studies, case series, or inconsistent results across trials. Insufficient indicates anecdotal reports, in-vitro data only, or no controlled human studies available. Sources include Cochrane Database of Systematic Reviews, PubMed-indexed clinical trials, and clinical guidelines from the American Academy of Dermatology, British Association of Dermatologists, and International Advisory Panel on Scar Management.Every effective scar treatment plan starts with a proper scar assessment. Whether you are evaluating a fresh surgical wound or an old mark that never fully faded, identifying your scar type is the single most important step before choosing a treatment. The interactive scar evaluation tool above walks you through four simple questions to classify your scar and match it with treatments ranked by clinical evidence. Below, you will find a detailed guide to each scar type, how dermatologists perform scar assessments in clinical settings, and what the research says about the most widely used treatments.
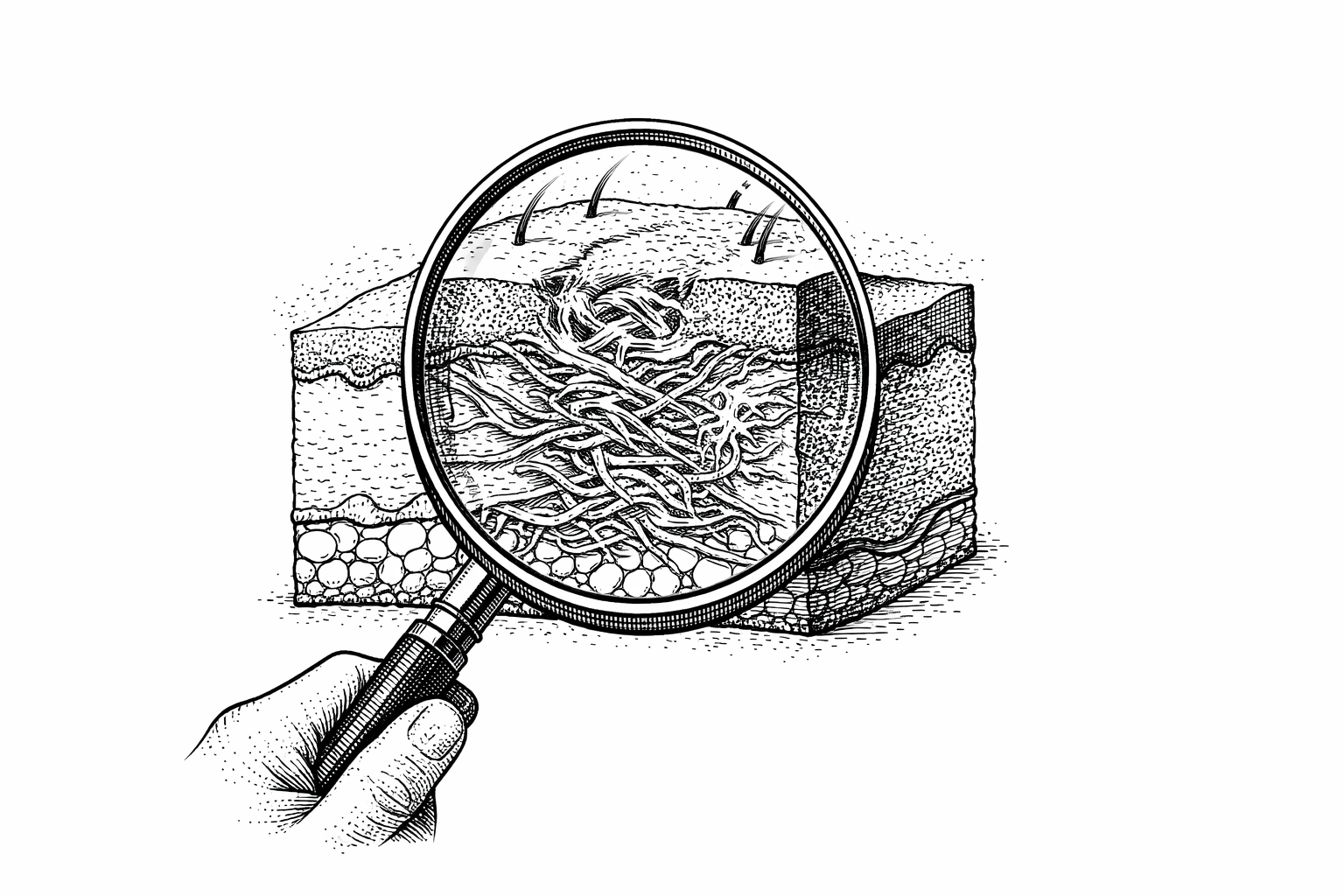
How to Assess Your Scar Type
Accurate scar assessment matters because each scar type involves distinct biological processes and responds to different interventions. A treatment that works well for one type may be ineffective — or even counterproductive — for another. When you evaluate your scar at home, the key characteristics to assess are whether the scar is raised above the surrounding skin, level with it, or depressed below it; whether it extends beyond the original wound boundary; and whether it restricts movement or causes ongoing symptoms like pain or itching.
Keloid scars
Keloid scars form when the body produces excess collagen that extends beyond the original wound boundary. They are more common in individuals with darker skin tones and frequently develop on the chest, shoulders, and earlobes. Unlike other raised scars, keloids do not resolve on their own and have high recurrence rates after surgical removal unless combined with adjuvant therapies such as corticosteroid injection or pressure therapy. If your scar assessment reveals a firm, raised mass that has grown larger than the original injury, a non-invasive keloid treatment plan or laser therapy for keloids may be appropriate starting points.
Hypertrophic scars
Hypertrophic scars also involve excess collagen production, but remain within the boundaries of the original wound. They are most common after burns, surgical incisions, and injuries in areas of high skin tension. Most hypertrophic scars improve gradually over 12 to 24 months, though some persist and require intervention. Approaches supported by clinical evidence include silicone sheeting, scar softening massage, and dermarolling for hypertrophic scars.
Atrophic scars
Atrophic scars sit below the normal skin surface, creating visible depressions or pits. They are the most common type of scar following acne and are classified into three subtypes: icepick scars, which are narrow and deep; boxcar scars, which are broad with defined edges; and rolling scars, which create a wave-like unevenness in the skin. Treatment selection depends heavily on the subtype and depth of the scarring. Microneedling therapy for atrophic scars and professional acne scar treatments are among the most clinically studied options.
Contracture scars
Contracture scars typically result from burns and are characterised by tight, thickened tissue that can restrict movement. When contractures affect joints or areas where skin flexibility is essential, they may require surgical intervention to restore function. Scar evaluation for contractures should include an assessment of range of motion and functional limitation, not just cosmetic appearance.
Flat (normotrophic) scars
Flat or normotrophic scars represent a normal healing outcome. The scar is level with the surrounding skin but may differ in colour or texture. Most flat scars continue to fade over 12 to 24 months. Sun protection during this period is one of the most strongly supported interventions for improving long-term appearance. If discolouration persists, dark scar fading methods and lightening serums for old scars may help.
Clinical Scar Assessment Scales: How Professionals Evaluate Scars
When dermatologists and plastic surgeons perform a formal scar evaluation, they typically use standardized assessment scales to measure scar severity and track improvement over time. Understanding the criteria these tools measure can help you evaluate your own scar more accurately before consulting a specialist — and give you the vocabulary to describe your scar during a clinical visit.
The Patient and Observer Scar Assessment Scale (POSAS) is one of the most widely used tools in scar research. It captures both the clinician’s objective assessment and the patient’s subjective experience across dimensions including colour, thickness, relief, pliability, surface area, and overall opinion. The Vancouver Scar Scale (VSS) is another established instrument that evaluates four characteristics — vascularity, height, pliability, and pigmentation — producing a composite severity score from 0 to 13. More recently, the SCAR-Q was developed to measure scar appearance, symptoms, and psychosocial impact in both children and adults aged eight and older.
These clinical scar assessment tools are designed for professional use, but the principles behind them apply to any self-evaluation. When you assess your scar, pay attention to color (is it red, pink, brown, or white compared to surrounding skin?), texture (smooth, rough, or uneven?), height (raised, flat, or depressed?), pliability (does the tissue move freely or feel stiff?), and any symptoms like pain, itching, or sensitivity. The interactive assessment at the top of this page uses similar criteria to help you classify your scar type and identify evidence-based treatment options.
How Scar Treatments Are Evaluated
Not all scar treatments are supported by the same quality of evidence. Clinical research ranges from large-scale randomized controlled trials, which provide the most reliable data, to small case series and anecdotal reports, which offer weaker support. The scar assessment tool above ranks treatments using this hierarchy so you can make informed decisions.
Treatments with strong evidence include silicone gel sheeting, which has been reviewed by the Cochrane Collaboration and recommended by the International Advisory Panel on Scar Management as a first-line option for both prevention and treatment of raised scars. Intralesional corticosteroid injection is another well-studied intervention, particularly for keloid and hypertrophic scars, with multiple randomized trials demonstrating reductions in scar volume and symptoms. Pressure therapy has strong evidence specifically in the context of burn scar management. For a broader look at topical options, see our guide to the best scar reduction creams.
Treatments with moderate evidence include fractional laser resurfacing, microneedling, cryotherapy, chemical peels, and dermal fillers. These interventions have been evaluated in controlled studies with generally positive outcomes, though the evidence base is smaller or less consistent than for first-line options.
Treatments with limited or insufficient evidence include many topical remedies commonly marketed for scar improvement. Vitamin E, aloe vera, tea tree oil, and onion extract have mixed or weak results across clinical studies. This does not necessarily mean they are ineffective, but rather that the current body of research does not yet provide reliable confirmation of their benefits.
Emerging research areas include recombinant protein therapies and advanced biomaterials designed to modulate the wound healing process at the cellular level. Early laboratory and observational data in these fields are promising, but published randomized controlled trials in humans remain limited. As formal clinical evidence develops, these approaches may offer new options for scar prevention and treatment.
When to Seek a Professional Scar Evaluation
While many scars improve with over-the-counter treatments and time, certain situations warrant a professional scar assessment. Scars that continue to grow beyond the original wound boundary, cause pain or persistent itching, restrict movement, or significantly affect quality of life should be evaluated by a board-certified dermatologist or plastic surgeon. Early intervention — particularly within the first 6 to 12 months of scar formation — is associated with better treatment outcomes across most scar types.
If you are unsure whether your scar needs professional attention, start with the interactive scar assessment tool above. It will help you identify your scar type and understand which treatments have the strongest evidence behind them. For scars following surgery, our guides to post-surgery scar care and when to apply scar cream after stitches cover the critical early recovery window in detail.




