Dermaroller for Scars: Before, After, and Everything In Between
Dermarolling for scars is one of the most searched skin treatments — and for good reason. Explore what the evidence shows about using a dermaroller for acne, surgical, and other scars.

What a Dermaroller Actually Does for Scars (And What the Evidence Shows)
Dermaroller for scars is one of the most searched skin treatment topics — and for good reason. Scars from acne alone affect up to 90% of people who experience acne vulgaris, and many of those marks persist long after the underlying condition resolves.
Here is a quick summary of what the evidence shows:
| Question | Evidence-Based Answer |
|---|---|
| Does it work? | Yes — clinical studies show meaningful scar improvement in the majority of patients |
| Best scar types | Atrophic scars (rolling, boxcar); less effective for ice pick or raised scars |
| Needle length for acne scars | 1.5 mm for deep dermal remodeling; 0.5–1.0 mm for milder surface scars |
| Sessions needed | Typically 3–4, spaced at least 6 weeks apart |
| When results appear | Gradual improvement over months; collagen remodeling continues for up to 6 months post-treatment |
| Main risks | Infection, post-inflammatory hyperpigmentation, improper technique at home |
| Professional vs. at-home | Professional treatment is safer and more effective; home use carries meaningful risks |
A dermaroller is a handheld device fitted with fine microneedles — typically 192 needles arranged in rows — that creates thousands of microscopic punctures in the skin when rolled across the surface. This controlled micro-injury triggers the skin's natural repair cascade: fibroblasts (the cells responsible for producing structural proteins) are activated, growth factors are released, and the body begins laying down new collagen and elastin.
This process is formally known as percutaneous collagen induction therapy (PCIT), or more broadly, microneedling.
The key distinction from more aggressive resurfacing treatments: the epidermis (the outermost skin layer) remains largely intact. Only the deeper dermis is disrupted — which means shorter recovery times and lower risk of post-procedure complications compared to ablative lasers or deep chemical peels.
That said, results are not instant, not guaranteed, and not equal across all scar types. The biology is real, but the clinical picture is nuanced.
This content is for informational purposes only and does not constitute medical advice. Consult a qualified healthcare professional for diagnosis and treatment.
How a Dermaroller for Scars Works: The Science of Microneedling
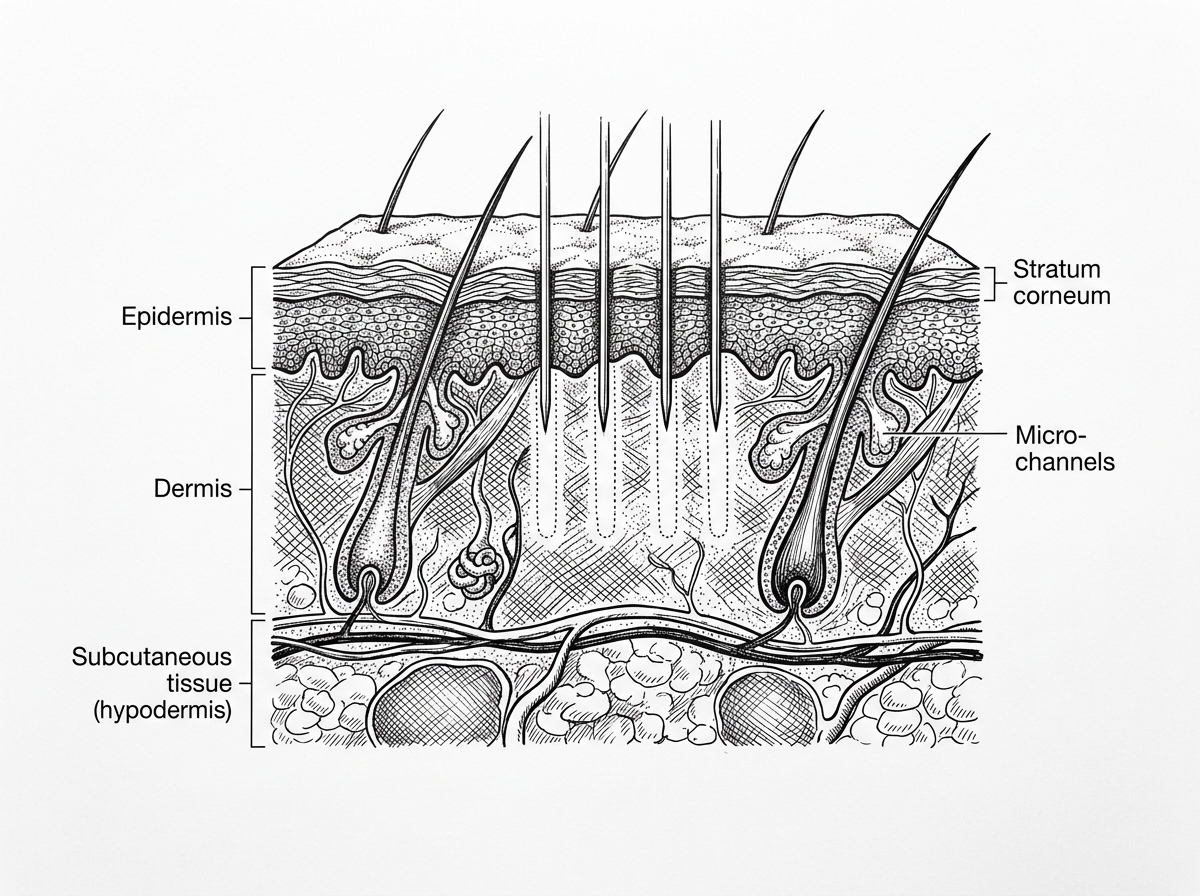
The biological foundation of using a dermaroller for scars rests on the skin’s innate ability to heal itself. When the microneedles penetrate the skin, they move through the stratum corneum (the outermost barrier) and enter the deeper dermis. This creates thousands of "micro-conduits" or tiny channels.
Research indicates that rolling a standard 192-needle device over a specific area 15 times results in approximately 250 holes per square centimeter. These punctures are microscopic, yet they are sufficient to cause localized "micro-trauma" without removing the protective epidermal layer.
The Three Stages of Dermal Remodeling
- Inflammation and Growth Factor Release: Immediately following the use of a dermaroller for scars, the body releases platelets and neutrophils. These cells produce essential growth factors, such as Transforming Growth Factor-beta (TGF-beta), Platelet-Derived Growth Factor (PDGF), and Fibroblast Growth Factor (FGF).
- Proliferation (Fibroblast Stimulation): Within hours, fibroblasts are recruited to the site of the micro-channels. These cells begin synthesizing a new extracellular matrix. A key feature of this stage is neovascularization—the formation of new blood vessels—which improves oxygen and nutrient delivery to the scarred tissue.
- Remodeling (Collagen III to Collagen I Conversion): Initially, the body lays down Type III collagen (the kind found in early wound healing). Over the following six months, this is slowly replaced by Type I collagen, which is stronger and more organized. Unlike the haphazard "spaghetti-like" arrangement of fibers in a scar, the new collagen aligns in a more natural, lattice-like structure, as noted in the Scientific research on microneedling principles.
This mechanical stimulation effectively "breaks up" the old, dormant scar tissue and replaces it with fresh, flexible tissue. Further details on this biological cascade can be found in our guide on Microneedling for Scar Reduction.
Effectiveness of the Dermaroller for Scars Across Different Tissue Types
While the dermaroller for scars is a versatile tool, its efficacy varies significantly depending on the nature of the scar tissue.
- Atrophic Scars: These are indentations caused by a loss of collagen (common in acne or chickenpox). This tissue type responds exceptionally well to microneedling because the treatment fills the "valleys" with new collagen.
- Hypertrophic Scars: These are raised, thickened scars. While microneedling can help soften the texture by breaking up dense fiber bundles, it must be used with caution to avoid triggering further overgrowth.
- Stretch Marks (Striae): These are essentially dermal tears. Clinical observations show that microneedling can improve the texture and "silvering" of stretch marks by inducing thick dermal remodeling.
- Surgical Adhesions and Burn Scars: Thicker, more restrictive scars often require longer needle lengths (up to 2.5 mm) to reach the deep fibrotic bands. Studies have shown significant improvement in mobility and texture for burn contractures after several sessions.
For a deeper dive into specific atrophic treatments, see Atrophic Scar Microneedling Therapy.
Using a Dermaroller for Acne Scars
Acne scarring is perhaps the most common application for this technology. In clinical settings, practitioners often use the Goodman-Baron quantitative scale to measure success.
Research shows that acne scars are typically categorized into three types:
- Ice Pick Scars (60% to 70%): Deep, narrow pits. These are the most difficult to treat with a dermaroller alone because the needles may not reach the very bottom of the narrow tract.
- Boxcar Scars (20% to 30%): Square-shaped indentations with sharp edges.
- Rolling Scars (15% to 25%): Shallow, wave-like undulations.
In a study by Fabbrocini et al., patients with rolling and boxcar scars saw the most significant improvement. Using a 1.5 mm needle length is generally considered the "gold standard" for these atrophic acne scars.
Recommended Needle Lengths for a Dermaroller for Scars
The depth of the scar dictates the length of the needle. Using a needle that is too short will fail to reach the fibroblasts, while a needle that is too long can cause unnecessary trauma.
| Needle Length | Primary Use | Target Layer |
|---|---|---|
| 0.2 mm - 0.3 mm | Product absorption | Stratum corneum |
| 0.5 mm | Shallow scars, fine lines, thin skin | Epidermal-Dermal junction |
| 1.0 mm | Moderate acne scars, light stretch marks | Papillary Dermis |
| 1.5 mm | Deep acne scars, surgical scars | Reticular Dermis |
| 2.0 mm - 2.5 mm | Deep body scars, thick burn tissue | Deep Dermis |
Practitioners often recommend starting with shorter lengths to assess skin tolerance before progressing to deeper dermal remodeling. More information on these variations can be found under Professional Treatment.
Professional Procedure, Technique, and Safety Protocols
A professional microneedling session follows a strict protocol to ensure both safety and efficacy. The process typically begins with the application of a topical anesthetic, such as EMLA cream (lidocaine/prilocaine), for 45 to 60 minutes. This is essential for needle lengths over 1.0 mm to ensure the procedure is comfortable.
The Rolling Technique
The "star" or "crosshatch" pattern is the standard method for ensuring even needle distribution. The practitioner rolls the device in four directions:
- Horizontal
- Vertical
- Diagonal (Left to Right)
- Diagonal (Right to Left)
The clinical endpoint of a successful session is "uniform pinpoint bleeding." This indicates that the needles have reached the papillary dermis, where the collagen-producing cells reside. Usually, 15 to 20 passes per area are required to achieve the necessary density of micro-channels.
Post-procedure, the skin will exhibit erythema (redness) similar to a mild sunburn, which typically lasts 2 to 3 days. Strict adherence to Scar Care protocols during this window is vital for healing. The FDA has issued safety communications regarding the risks of microneedling, emphasizing that devices should be used by trained professionals to avoid "tram track" scarring or infection—see the FDA safety communication for more.
At-Home Risks and Sterilization Requirements
While at-home dermarolling has become popular, it carries significant risks if not performed with surgical-level hygiene.
- Sterilization: The device must be soaked in 70% isopropyl alcohol for at least 5–10 minutes before and after every use. CDC guidelines for disinfection emphasize that simple hot water is insufficient to kill pathogens that can cause staph infections or cellulitis.
- Needle Integrity: Home rollers often use cheap, "flower-shaped" stamped metal rather than individual medical-grade needles. These can hook or "tear" the skin rather than piercing it, leading to permanent "tram track" scarring.
- Dulling: Needles become blunt after just a few uses. A dull needle requires more pressure, which increases the risk of tissue tearing.
- Cross-contamination: Rolling over active acne, cold sores (Herpes Simplex), or warts can spread the infection across the entire face.
Clinical Comparisons: PRP, Copper Peptides, and Adjunct Therapies
Evidence suggests that while a dermaroller for scars is effective as a monotherapy, combining it with other substances can enhance results.
The PRP Advantage
Platelet-Rich Plasma (PRP) involves drawing a patient's blood, concentrating the platelets, and applying the resulting serum to the skin during or after microneedling. A split-face study showed that while 92% of patients had a "fair" response to dermarolling alone, 80% had a "good" response and 20% had an "excellent" response when PRP was added. The growth factors in PRP act as a "turbo-charge" for the healing process. You can read more about this in the Study comparing dermaroller and PRP.
Copper Peptides (GHK-Cu)
Copper peptides are naturally occurring complexes that promote wound healing and stimulate matrix metalloproteinase-2. A study of 40 patients showed that adding copper peptides to a dermaroller regimen reduced scar scores by 6 points, compared to 4.5 points for the dermaroller alone. However, the study also noted a 40% risk of temporary hyperpigmentation in the combination group, suggesting that monotherapy might be safer for those with darker skin tones (Fitzpatrick types IV-V).
For a comparison of these methods versus light-based therapies, see our Laser Treatment for Scars Complete Guide.
Combining Treatments with a Dermaroller for Scars
Practitioners often use a "multimodal" approach for complex scarring:
- Subcision: For "tethered" rolling scars, a needle is used to break the fibrous bands pulling the skin down. Microneedling is then performed to smooth the surface.
- Chemical Peels: Alternating microneedling with light chemical peels can improve surface pigmentation and texture.
- Vitamin C (L-ascorbic acid): Applying Vitamin C post-needling can enhance collagen synthesis, though it must be a stable, non-irritating formulation to avoid "granulomas" (tiny inflammatory bumps).
Learn more about these synergistic approaches in our guide on Quick Scar Fading Treatment.
Frequently Asked Questions about Dermarolling
How many sessions are needed for visible results?
Most clinical studies involve a series of 3 to 4 treatments. Because collagen remodeling is a slow biological process, sessions should be spaced at least 6 weeks apart. This allows the skin to complete the inflammatory and proliferative phases of healing. While some initial "plumping" (due to edema) is visible within a week, the true results—permanent dermal thickening—are typically assessed at the six-month mark post-treatment. This is supported by research on long-term efficacy.
What are the primary contraindications for treatment?
One should avoid using a dermaroller for scars if they have:
- Active acne or skin infections (to prevent bacterial spread).
- A history of keloidal (excessive) scarring.
- Herpes Simplex (cold sore) outbreaks in the treatment area.
- Used isotretinoin (Accutane) within the last 6 to 12 months (as it impairs wound healing).
- Immunosuppressive disorders or uncontrolled diabetes.
General advice on when to seek alternatives can be found at Scar Treatment.
What post-procedure care is required?
The 48 hours following treatment are critical. The skin barrier is temporarily compromised, making it highly sensitive.
- Photoprotection: Strict sun avoidance and a physical SPF 30+ sunscreen are mandatory. UV exposure on "open" skin can lead to permanent post-inflammatory hyperpigmentation.
- Hydration: Use only gentle, non-comedogenic moisturizers or hyaluronic acid.
- Avoid Actives: Do not use retinoids, Vitamin C, or AHAs/BHAs for at least 3–5 days, as these can cause severe irritation.
- Cleanliness: Use saline compresses if the skin feels tight or crusty, and avoid touching the face with unwashed hands.
For more on maintaining your results, see Scar Fading.
Conclusion
The use of a dermaroller for scars is a scientifically validated method for improving skin texture and reducing the visibility of atrophic marks. By harnessing the body’s natural percutaneous collagen induction process, it offers a middle ground between superficial topicals and aggressive laser surgeries.
However, success is highly dependent on using the correct needle length, maintaining a sterile environment, and having realistic expectations. While a 50-70% improvement in scar depth is a common clinical outcome, "perfect" skin is rarely achievable. For those dealing with specific areas, such as the lower limbs, our resource on Microneedling for Ankle Scars provides targeted advice.
Whether performed in a clinic or carefully at home, microneedling remains a cornerstone of modern scar management. For further reading and updates on the latest techniques, explore More info on microneedling.
This content is for informational purposes only and does not constitute medical advice. Consult a qualified healthcare professional for diagnosis and treatment.




