An Essential Guide to Surgical Scar Revision
Surgical Scar Revision: Clinical Definition and Pathophysiological Overview
Surgical scar revision is a set of operative and adjunctive procedures designed to improve the appearance, function, or symptoms of a scar — though it cannot erase a scar entirely.
For anyone living with a visible scar from an injury, surgery, burn, or skin condition, here is what the evidence shows:
| Question | Evidence-Based Answer |
|---|---|
| Can surgery remove a scar completely? | No. Revision improves appearance and function; the scar remains but becomes less conspicuous. |
| Who is it for? | Those with mature scars causing functional impairment, significant cosmetic distress, or pain. |
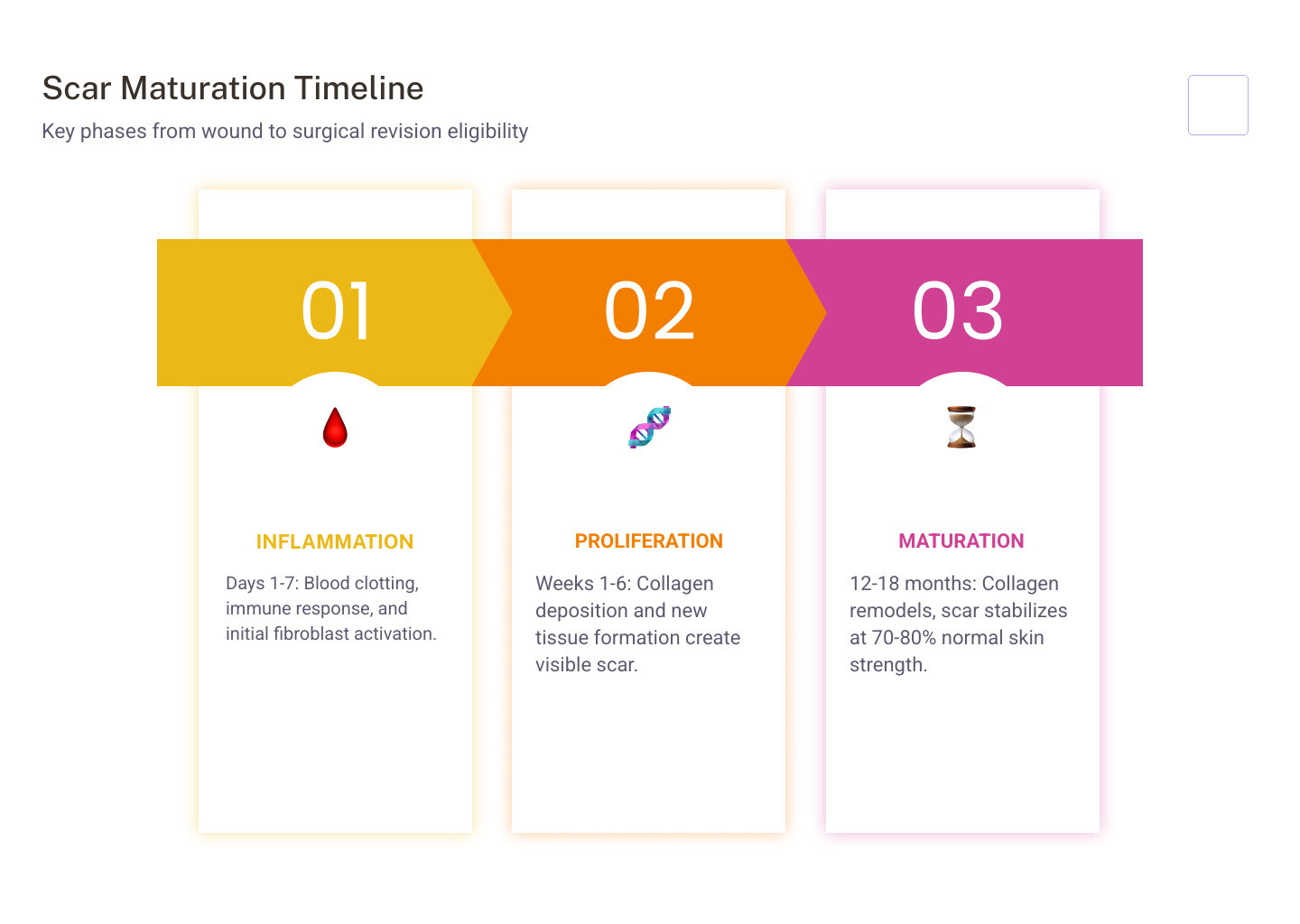
| When can revision be done? | Generally after 12–18 months, once the scar has fully matured. |
| What techniques are used? | Z-plasty, W-plasty, elliptical excision, skin grafts, tissue expansion, and adjunct therapies. |
| Is surgery always needed? | No. Topical treatments, injectables, and laser therapy are first-line for many scar types. |
Scars are an unavoidable consequence of the body's wound-healing process. When the deeper layer of skin — the reticular dermis — is disrupted, the body repairs the damage with fibrous collagen tissue rather than regenerating the original skin architecture. The result is a scar: structurally functional, but visually and sometimes physically distinct from the surrounding skin.
For most people, scars fade gradually over time. Research indicates that a scar typically reaches maturity — meaning its collagen structure has stabilized and its tensile strength has approached roughly 70–80% of uninjured skin — somewhere between 12 and 18 months after the initial wound. Before that point, the tissue is still actively remodeling, and surgical intervention is generally less likely to yield optimal results.
When scars remain raised, contracted, pigmented, or functionally limiting after that maturation window, surgical revision becomes a clinically relevant option.
This guide reviews the science behind surgical scar revision: the biological mechanisms that drive scar formation, the clinical indications for surgery, the techniques surgeons use, how to prepare, what recovery involves, and what realistic outcomes look like — drawing on peer-reviewed research and established clinical guidelines.
Clinical Indications and Pathophysiological Classification of Scars
The decision to proceed with surgical scar revision depends heavily on the scar's classification. Not all scars respond equally to surgical intervention, and some may even worsen if the surgical approach is inappropriate for the tissue type. Clinical assessment typically utilizes tools like the Vancouver Scar Scale to evaluate vascularity, pigmentation, pliability, and height.
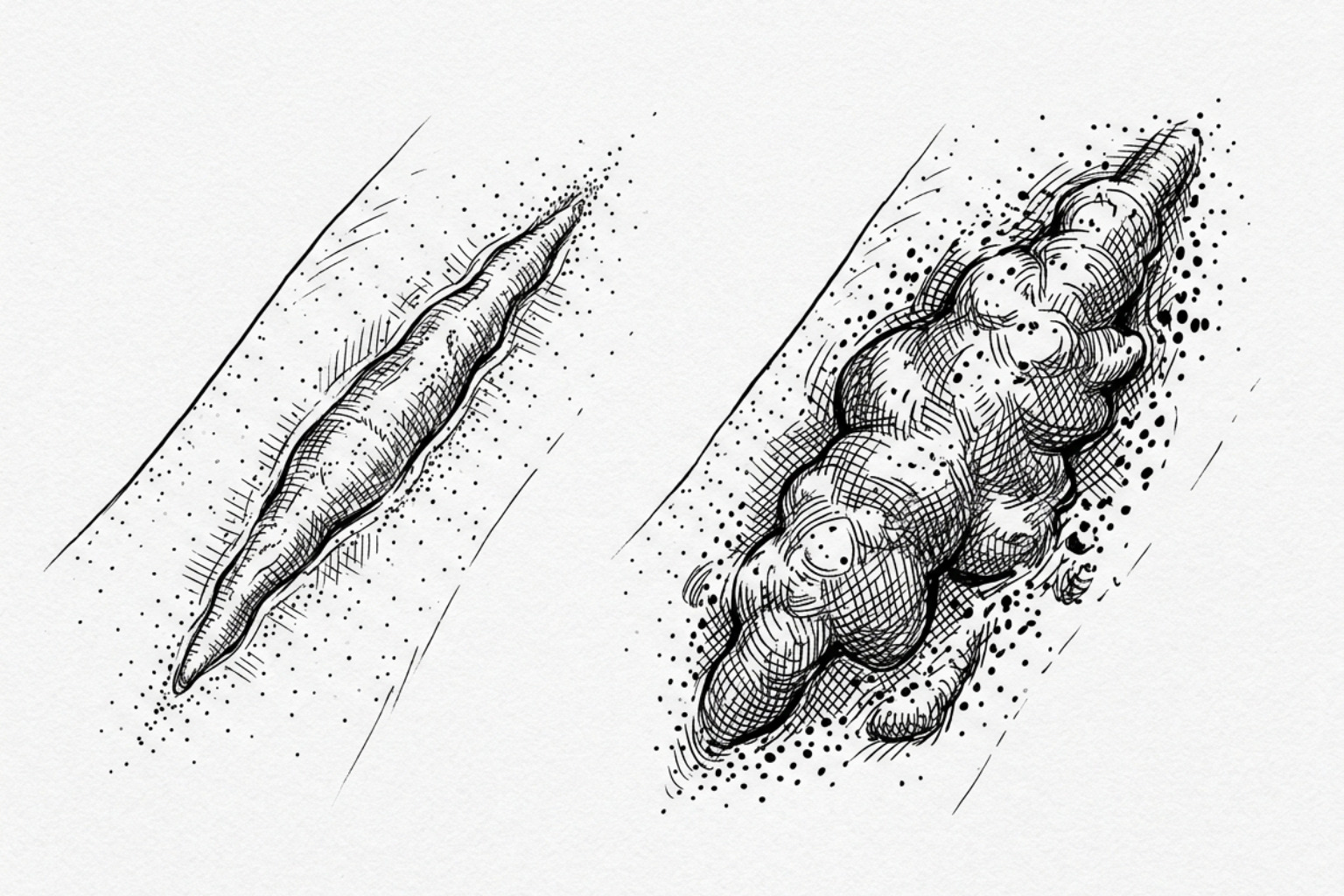
Pathophysiology of Hypertrophic and Keloid Scars
The biological foundation of problematic scarring lies in the behavior of fibroblasts, the cells responsible for synthesizing collagen. When the inflammatory phase of wound healing is prolonged or excessive, fibroblasts overproduce collagen fibers, which become disorganized in the reticular dermis.
- Hypertrophic Scars: These are raised, red, and firm. They remain within the boundaries of the original wound and often develop within weeks of the injury. While they may improve naturally over a year or more, surgery is considered if they remain symptomatic or unsightly after maturation.
- Keloid Scars: These represent a more aggressive form of scarring. Keloids extend beyond the original wound margins and can appear up to one year after the trauma. They are more common in individuals with darker skin tones and frequently occur in areas with little underlying fatty tissue, such as the ears, chest, and shoulders. Surgical removal of keloids carries a high risk of recurrence, often requiring multimodal therapy, such as laser for keloid scars.
Functional vs. Aesthetic Revision
While many patients seek revision for cosmetic reasons, surgery is often medically indicated for functional impairment.
- Contractures: These occur when a large area of skin is lost (often from burns) or when a wound crosses a joint. The resulting scar tissue pulls the skin edges together, restricting the movement of muscles, joints, and tendons.
- Atrophic Scars: These are depressed or "pitted" scars, often resulting from acne or infections where underlying fat or muscle is lost.
- Facial Symmetry: Scars that distort features—such as the eyelid (causing ectropion) or the lip—require surgical repositioning to restore both form and function.
In cases where the scar is hard or restrictive, clinicians may recommend scar tissue massage therapy as a non-surgical adjunct to improve pliability before or after surgery.
Procedural Methodologies in Reconstructive Scar Surgery
The primary goal of surgical scar revision is to reorient the scar so that it aligns with the Relaxed Skin Tension Lines (RSTLs). These are the natural folds and wrinkles of the skin. A scar that runs parallel to these lines is significantly less visible than one that crosses them.
Geometric Logic of Z-plasty and W-plasty in Surgical Scar Revision
Surgeons use geometric patterns to "break up" a straight-line scar, making it harder for the eye to track and reducing the tension on the tissue.
- Z-plasty: This is the most common technique for elongating a contracted scar or reorienting its direction. By creating two triangular flaps, the surgeon rotates the tissue. A standard 60-degree Z-plasty can provide a 75% gain in tissue length and a 90-degree change in the scar's direction.
- W-plasty: This technique involves creating a series of small triangular incisions along the scar's edges. When closed, the resulting "zig-zag" line reflects light irregularly, making the scar less conspicuous. Unlike Z-plasty, W-plasty does not lengthen the scar but is excellent for irregularizing linear scars on the face.
- Elliptical Excision: For simple, narrow scars, the surgeon may perform a fusiform (oval) excision. To prevent "dog-ear" puckering at the ends, the length-to-width ratio is typically kept at 3:1, with end angles of 30 degrees or less.
For those interested in enhancing the results of these excisions, co2 laser for surgical scars before and after studies show that laser resurfacing can further blend the revised edges with surrounding skin.
Skin Grafts, Flaps, and Tissue Expansion
When a scar is too large for simple excision, more complex reconstructive methods are required.
- Skin Grafts: Healthy skin is taken from a donor site and attached to the revision area. While functional, grafts may not perfectly match the color or texture of the surrounding skin.
- Skin Flaps: Similar to grafts, but the donor tissue remains attached to its own blood supply. This is preferred for areas with poor vascularization.
- Tissue Expansion: This involves placing a silicone balloon under the skin near the scar. Over several weeks, the balloon is filled with salt water, gradually stretching the healthy skin to create enough "extra" tissue to cover the area once the scar is excised.
These advanced methods are often followed by laser treatment for surgical scars to optimize the final texture.
Preoperative Assessment and Patient Selection Criteria
Successful surgical scar revision begins long before the first incision. Patient selection is critical because systemic health directly impacts the quality of the final scar.
Patient Selection and Timing for Surgical Scar Revision
The most important factor in timing is scar maturity. Operating on an "immature" scar—one that is still red, itchy, or firm—is a significant risk factor for poor outcomes and hypertrophic recurrence. Most experts recommend waiting 12 to 18 months post-injury.
Preparation requires strict lifestyle adjustments:
- Smoking Cessation: Patients must be smoke-free for at least 30 days before surgery. Tobacco use impairs microcirculation and significantly increases the risk of wound dehiscence (opening) and infection.
- Nutritional Optimization: Wound healing requires specific building blocks. A diet rich in Zinc and Vitamins A, C, and E is clinically recommended to support collagen synthesis and immune function.
- Glucose Control: For diabetic patients, maintaining blood glucose levels below 180 mg/dL is essential to prevent healing delays.
Patients should also be educated on when to apply scar cream after stitches are removed to support the new incision's healing.
Contraindications and Risk Factors
Surgery may not be recommended for individuals with:
- Uncontrolled comorbidities like severe diabetes or autoimmune disorders.
- Active skin infections in the surgical field.
- A history of multiple failed keloid revisions (where surgery might trigger even larger keloid growth).
- Current use of anticoagulants (blood thinners) that cannot be safely paused for the procedure.
Postoperative Management and Complication Mitigation Protocols
The surgery only creates a "new" wound; the final appearance of the scar is determined by the care provided during the months of recovery.
Optimizing the Maturation Phase
The goal of post-surgery scar care is to minimize tension and inflammation.
- Silicone Therapy: Silicone gel sheets or gels are the gold standard for non-invasive postoperative care. They should be used 12 to 24 hours daily for several months. They work by hydrating the stratum corneum and reducing fibroblast activity.
- Pressure Therapy: For patients prone to keloids, pressure appliances may need to be worn day and night for 4 to 6 months.
- Sun Protection: Healing scars are highly susceptible to permanent hyperpigmentation (tanning). Strict use of broad-spectrum sunscreen and physical covering is required for at least one year.
If the new scar feels firm, techniques for hard scar softening massage may be introduced once the incision is fully closed.
Managing Complications and Recurrence
Even with perfect technique, complications can occur.
- Infection and Hematoma: These require immediate clinical attention to prevent total wound failure.
- Hypertrophy Recurrence: If a scar begins to thicken, intralesional steroid injections (triamcinolone) are often used. However, research indicates that up to 63% of patients experience adverse effects from steroids, such as skin thinning or visible blood vessels.
- Cryotherapy: Intralesional cryotherapy (freezing the tissue from the inside) is another option, though it has a 75% adverse effect rate, including permanent pigment loss.
In many cases, surgical scar laser treatment or co2 laser scar removal is preferred for managing early signs of thickening or redness.
Comparative Efficacy: Surgical Intervention versus Non-Invasive Modalities
Surgical scar revision is often the "last resort" or a component of a multimodal plan. The following table summarizes how surgery compares to common non-invasive treatments.
| Modality | Primary Use | Effectiveness | Key Limitation |
|---|---|---|---|
| Surgical Excision | Narrowing wide scars, reorienting tension | High for mechanical issues | Creates a new scar |
| Laser Resurfacing | Texture, color, and minor height issues | 20–60% contraction | Requires multiple sessions |
| Steroid Injections | Flattening raised scars | 50–100% (variable) | High risk of skin atrophy |
| Chemical Peels | Superficial pigment and fine texture | Moderate for surface | Not for deep/raised scars |
The Role of Laser Resurfacing and Dermabrasion
For many patients, a combination of surgery and laser therapy yields the best results. A Pulsed Dye Laser is effective for reducing the redness of a new scar, while ablative lasers like CO2 induce collagen remodeling and wound contraction. For a deeper look at these options, refer to the laser treatment for scars complete guide.
Dermabrasion—mechanically sanding the skin—is often performed 6 to 8 weeks after a surgical revision to "blur" the edges of the new scar into the surrounding skin. Similarly, chemical peel scar revision can be used for very superficial irregularities.
Injectables and Soft Tissue Fillers
For atrophic (depressed) scars, surgery may be avoided in favor of fillers.
- Fat Grafting: Using the patient's own fat to provide long-lasting volume.
- Hyaluronic Acid: Temporary fillers that can lift "pockmarks" or acne scars.
- 5-Fluorouracil (5-FU): A chemotherapy agent sometimes injected alongside steroids to prevent the recurrence of hypertrophic tissue with fewer side effects than steroids alone.
Clinical Considerations and Patient Consultation Parameters
Can surgical revision completely remove a scar?
No. There is currently no medical technology that can return scarred skin to its original, uninjured state. Surgery replaces an unsightly or restrictive scar with a thinner, flatter, and better-positioned one.
How long is the recovery period after scar surgery?
Initial healing (stitch removal) takes 3 to 7 days. However, the "biological" recovery takes much longer. The scar will look red and perhaps worse for the first few weeks, only beginning to fade and soften after 3 to 6 months. The final result is not visible for at least a year.
Why must I wait a year before seeking surgical revision?
The body is a busy construction site for the first 12 months after an injury. If a surgeon operates while the tissue is still remodeling, the risk of the body overreacting and creating a larger, thicker scar is significantly higher. Patience allows the tissue to stabilize, ensuring the revision is performed on a "quiet" foundation.
Summary and Clinical Outlook
Surgical scar revision is a powerful tool for restoring function and improving the quality of life for those with significant scarring. However, it is not a "magic eraser." Success requires a combination of precise surgical technique, such as Z-plasty or W-plasty, and diligent postoperative care involving silicone therapy and sun protection.
By understanding the 12–18 month maturation timeline and the importance of preoperative health, patients can set realistic expectations for their outcomes. Whether through surgery, laser treatment, or adjunctive therapies, the goal remains the same: a scar that is less conspicuous and a body that moves without restriction.
To understand your specific scar type and the best path forward, you can start your personalized scar assessment.
Works Cited
- "Scar Revision." StatPearls [Internet]. National Center for Biotechnology Information. https://www.ncbi.nlm.nih.gov/books/NBK542318/
- "Surgical Scar Revision: An Overview." Journal of Cutaneous and Aesthetic Surgery. https://ncbi.nlm.nih.gov/pmc/articles/PMC3996787/
- "Scar revision." MedlinePlus Medical Encyclopedia. https://www.medlineplus.gov/ency/article/002991.htm
- "Scar Revision: What It Is, Who Is a Candidate and Treatment Options." Cleveland Clinic.
- "Scar Revision." Johns Hopkins Medicine.
This content is for informational purposes only and does not constitute medical advice. Consult a qualified healthcare professional for diagnosis and treatment.




