Medicine Cabinet Makeover: Get Rid of Pimples and Dark Spots

Clinical Management of Acne Vulgaris and Associated Post-Inflammatory Hyperpigmentation
Skin care for pimples and dark spots addresses two distinct but closely linked biological processes: active acne (acne vulgaris) and the post-inflammatory hyperpigmentation (PIH) that frequently follows. According to the American Academy of Dermatology, PIH is a common consequence of inflammatory skin conditions and requires a targeted therapeutic approach.
Here is a concise overview of the most clinically supported approaches:
| Concern | Key Ingredients | Evidence Level |
|---|---|---|
| Active pimples | Salicylic acid, benzoyl peroxide, adapalene | Strong (clinical guidelines) |
| Dark spots (PIH) | Niacinamide, azelaic acid, tranexamic acid, vitamin C | Moderate to strong |
| Both simultaneously | Retinoids, glycolic acid, kojic acid | Moderate |
| Prevention | Broad-spectrum SPF 30+ daily | Strong |
Acne is one of the most common skin conditions globally. For many individuals—particularly those with higher Fitzpatrick skin types—the inflammatory lesion is often followed by flat, darkened patches that can persist for months. These marks are distinct from structural scars; PIH is a pigmentary response where the skin produces excess melanin during the healing process.
Research indicates that atrophic scars affect between 80 and 90% of people with acne, and PIH is disproportionately common in individuals with melanin-rich skin tones. This article reviews the biology behind both conditions, the ingredients with the strongest clinical evidence, and the structure of a daily routine designed to address active breakouts and lingering pigmentation simultaneously.

Pathophysiology of Acne Vulgaris and Post-Inflammatory Hyperpigmentation
The development of a pimple is a multi-stage inflammatory process. According to the British Journal of Dermatology, acne vulgaris typically involves four primary factors: excess sebum (oil) production, follicular hyperkeratinization (clumping of dead skin cells), the presence of Cutibacterium acnes bacteria, and inflammation.
When a pore becomes blocked, an inflammatory response is triggered. This inflammation does more than just cause redness and swelling; it serves as a signal to melanocytes, the pigment-producing cells located at the base of the epidermis. In response to inflammatory cytokines, these melanocytes increase the production of melanin and transfer it to surrounding skin cells (keratinocytes) via small packages called melanosomes.
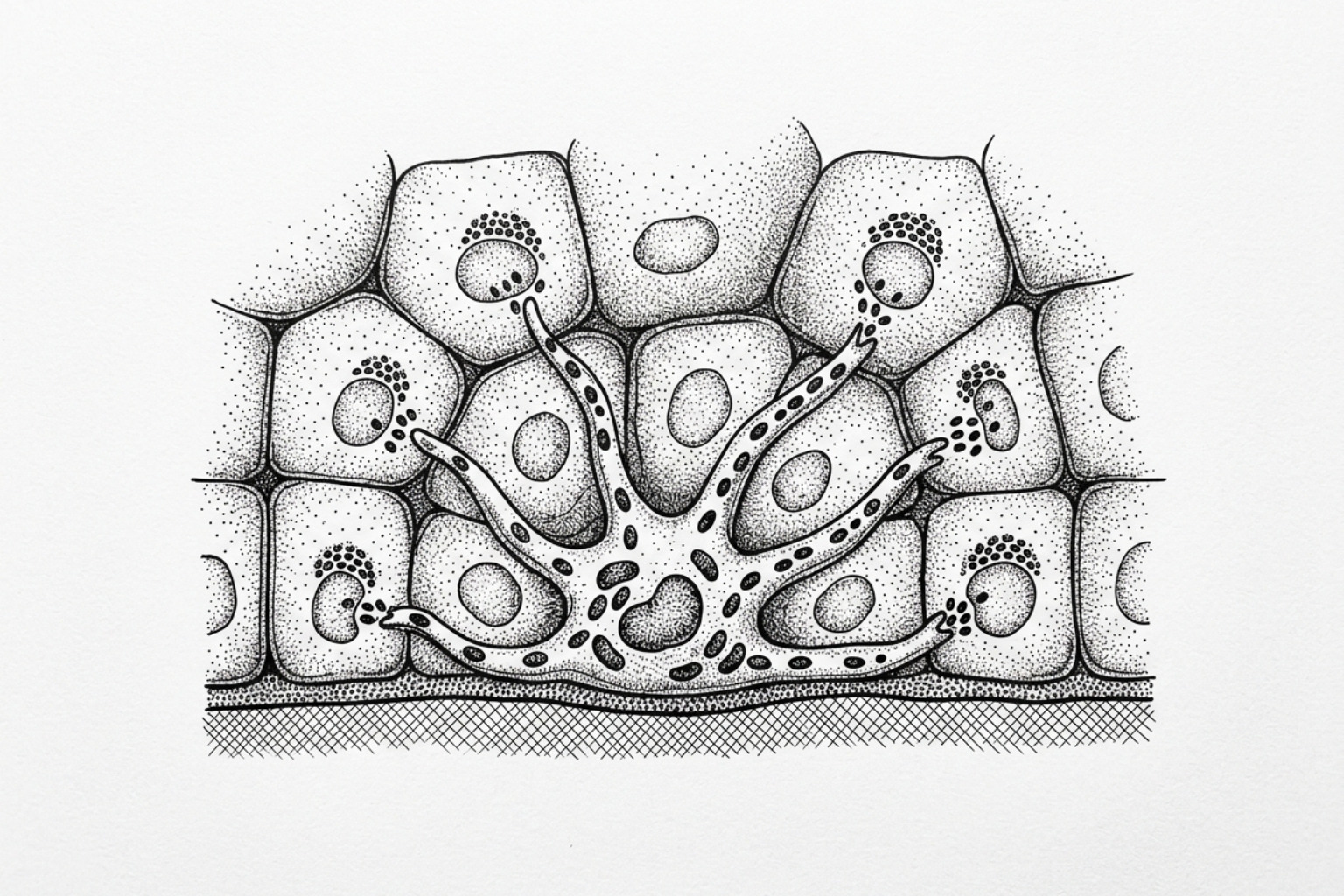
This process results in Post-Inflammatory Hyperpigmentation (PIH). The depth of the pigment determines how long the spot lasts. Epidermal PIH, where the melanin is trapped in the top layer of skin, typically appears brown or tan and may take 6 to 12 months to resolve. Dermal PIH occurs when pigment "leaks" into the deeper dermis; these spots often appear blue-gray or deep purple and can persist for years without clinical intervention.
Clinical Classification of Post-Acne Marks and Atrophic Scarring
It is clinically vital to distinguish between pigmentary changes and structural scarring. Many individuals refer to dark spots as "scars," but they are biologically distinct.
Pigmentary Changes (Non-Structural)
- Post-Inflammatory Hyperpigmentation (PIH): Flat, brown, or black spots caused by excess melanin.
- Post-Inflammatory Erythema (PIE): Flat, red, or pink marks caused by dilated capillaries near the skin surface, most common in lighter skin tones.
Atrophic and Hypertrophic Scars (Structural)
When the skin’s healing process is disrupted, it may result in a loss of collagen (atrophic) or an overproduction of fibrous tissue (hypertrophic).
- Ice Pick Scars: Narrow, deep "holes" that extend into the dermis.
- Boxcar Scars: Round or oval depressions with sharp, vertical edges.
- Rolling Scars: Wide depressions that create an undulating, "wave-like" appearance on the skin.
- Keloids: Raised, thick scars that grow beyond the boundary of the original injury.
Understanding these differences is the first step in selecting the best scar reduction cream or treatment. While PIH can be managed with topical brighteners, atrophic scars often require professional procedures like microneedling or laser resurfacing. For more detailed guidance, explore resources on pimple scar removal cream and how to tag acne scars for identification.
| Feature | PIH / PIE | Atrophic Scars | Hypertrophic Scars |
|---|---|---|---|
| Texture | Flat / Smooth | Pitted / Indented | Raised / Firm |
| Cause | Melanin or blood flow | Collagen loss | Excess collagen |
| Resolution | Fades over time | Permanent without treatment | May soften but persists |
Evidence-Based Skin Care for Pimples and Dark Spots: Active Ingredients
To effectively manage skin care for pimples and dark spots, ingredients must target both the bacterial/inflammatory source of the acne and the enzymatic pathways of pigment production. A review in the Journal of Clinical and Aesthetic Dermatology emphasizes that successful treatment of PIH requires both the resolution of the underlying inflammation and the inhibition of melanogenesis.
- Salicylic Acid (BHA): A lipid-soluble acid that penetrates pores to dissolve sebum and dead skin cells. Research shows it is highly effective for comedonal acne and provides mild exfoliation to help fade surface spots.
- Benzoyl Peroxide: An antimicrobial agent that reduces C. acnes populations. Clinical data suggests that lower concentrations (2.5%) are often as effective as 10% but with significantly less irritation.
- Azelaic Acid: A dicarboxylic acid that treats both concerns simultaneously. It is antimicrobial and anti-inflammatory, while also acting as a tyrosinase inhibitor to block melanin production.
- Niacinamide (Vitamin B3): This ingredient stabilizes the skin barrier and inhibits the transfer of melanosomes to skin cells. It is a cornerstone of dark scar removal methods due to its high tolerability.
Topical Retinoids and Alpha Hydroxy Acids
Retinoids and Alpha Hydroxy Acids (AHAs) accelerate cell turnover, facilitating the desquamation of pigmented keratinocytes.
- Adapalene: A third-generation retinoid that regulates cell turnover and prevents the formation of new microcomedones.
- Glycolic Acid: An AHA with a small molecular size for deep penetration. It dissolves the intercellular adhesions of dead skin cells, improving texture and fading surface discoloration.
- Lactic Acid: A gentler AHA that also acts as a humectant, making it suitable for sensitive skin types seeking an old scar lightening serum effect.
Tyrosinase Inhibitors and Anti-Inflammatory Agents
Specialized brighteners are required to halt the overproduction of pigment.
- Tranexamic Acid: Topically, it interferes with the pathway between melanocytes and keratinocytes, particularly in UV-induced pigmentation.
- Vitamin C (L-Ascorbic Acid): An antioxidant that neutralizes free radicals and inhibits tyrosinase.
- Licorice Root Extract: Contains liquiritin, which helps disperse existing melanin, and glabridin, which inhibits UV-induced pigmentation.
- Kojic Acid: A well-documented tyrosinase inhibitor often used in quick scar fading treatment protocols.
Designing a Therapeutic Routine for Active Acne and Pigmentation
A successful routine must balance "attack" (actives) with "defense" (barrier support). Over-treating the skin with excessive acids can compromise the skin barrier, increasing inflammation and potentially worsening PIH.
The Role of Sun Protection
Sunscreen is the most critical component of any PIH treatment plan. UV radiation stimulates melanocytes to produce more pigment. Without broad-spectrum SPF 30 or higher, topical brighteners will be largely ineffective, as UV exposure will continually darken the areas of hyperpigmentation.
Barrier Support
Ingredients like ceramides, squalane, and hyaluronic acid are vital. They ensure the skin remains hydrated and the lipid barrier intact while using potentially drying agents like benzoyl peroxide or retinoids.
Formulating a Daily Skin Care for Pimples and Dark Spots
A standard evidence-based routine might include:
Morning (Focus: Protection & Prevention)
- Gentle Cleanser: Removes overnight oils without stripping the skin.
- Vitamin C or Niacinamide Serum: Provides antioxidant defense and initiates the brightening process.
- Oil-Free Moisturizer: Essential for all skin types to prevent compensatory oil production.
- Broad-Spectrum Sunscreen (SPF 30+): The non-negotiable step for fading spots.
Evening (Focus: Treatment & Repair)
- Cleanser: Removes daily pollutants and sunscreen.
- Active Treatment: Apply a thin layer of a retinoid (like adapalene) or an exfoliating acid (like salicylic or glycolic acid). Note: These should not be used simultaneously to avoid irritation.
- Targeted Brightener: Apply a serum containing azelaic acid or tranexamic acid to specific dark spots.
- Barrier-Restoring Moisturizer: Products containing ceramides help soothe the skin overnight. This is often the best scar reduction cream approach for maintaining skin health.
Specialized Skin Care for Pimples and Dark Spots in Melanated Skin
Individuals with skin of color (Fitzpatrick types IV-VI) require specific considerations. Melanocytes in darker skin are more reactive, meaning minor irritation can trigger significant PIH.
- Avoid Physical Exfoliants: Scrubbing can cause micro-tears and inflammation, leading to further hyperpigmentation.
- Pomade Acne: Acne along the hairline is often caused by oils in hair products. Switching to water-based products can resolve this specific type of breakout.
- Keloid Awareness: Darker skin tones have a higher genetic predisposition to keloid scarring. Early intervention for cystic acne is crucial to prevent these raised scars.
- Tyrosinase Sensitivity: Ingredients like kojic acid and alpha-arbutin are often preferred over hydroquinone for long-term use in skin of color to avoid the risk of exogenous ochronosis.
For more on managing these specific needs, see the tag for scar fading.
Clinical Expectations and Common Therapeutic Errors
Patience is the most difficult part of skin care for pimples and dark spots. Skin cells take approximately 28 to 40 days to turn over. Therefore, any treatment requires at least three cell cycles — roughly three months — to show significant results.
Common Mistakes
- Picking and Popping: This increases the depth of the wound and the level of inflammation, almost guaranteeing a darker, longer-lasting spot or a permanent atrophic scar.
- Inconsistency: Using a treatment "here and there" will not yield results. Pigment inhibition must be constant.
- Skipping Sunscreen on Cloudy Days: UVA rays, which contribute to pigmentation, penetrate clouds and glass.
- Over-Exfoliating: If your skin is peeling, red, or stinging, you are likely causing more inflammation, which will lead to more PIH.
If topical treatments do not show improvement after 3 months, or if you are experiencing deep, painful cysts, it is time to seek a dermatologist. They can provide prescription-strength retinoids, chemical peels, or laser treatments that penetrate more deeply than over-the-counter options. You can also reduce acne scars fast by combining professional advice with a solid home routine.
Frequently Asked Questions about Acne and Pigmentation
How long does it take for post-acne dark spots to fade?
Epidermal (surface) dark spots typically take 6 to 12 months to fade naturally. With consistent use of active ingredients like retinoids and tyrosinase inhibitors, this timeline can often be reduced to 3 to 6 months. Dermal (deep) spots may take years to resolve without professional intervention.
Can topical creams fix pitted acne scars?
Topical creams are generally ineffective at "filling in" pitted or atrophic scars like ice pick or boxcar scars. These scars involve a loss of collagen in the deeper dermis. While retinoids can slightly improve skin texture over time, structural changes usually require clinical procedures like subcision, laser resurfacing, or fillers.
Why do dark spots get darker after sun exposure?
Dark spots are areas of concentrated melanin. UV radiation acts as a direct stimulant for melanocytes. When exposed to the sun, these cells produce even more melanin as a defense mechanism, making existing hyperpigmentation significantly darker and more difficult to treat.
Conclusion
Managing skin care for pimples and dark spots is a long-term process. By understanding the inflammatory cascade that leads from a blemish to a dark spot, individuals can intervene effectively using evidence-based ingredients like salicylic acid, azelaic acid, and retinoids.
The foundation of any successful regimen is protection. Daily sun protection, gentle cleansing, and consistent application of active ingredients are the keys to achieving a clearer, more even complexion. While pigment may fade over time, structural scars require a different clinical approach.
Start your personalized scar assessment today to find the best path forward for unique skin needs.
Works Cited
- American Academy of Dermatology. "Acne Scars: Signs and Symptoms."
- Journal of Clinical and Aesthetic Dermatology. "Postinflammatory Hyperpigmentation: A Review of the Epidemiology, Clinical Features, and Treatment Options in Skin of Color."
- Mayo Clinic. "Acne: Diagnosis and Treatment."
- British Journal of Dermatology. "The Pathogenesis of Acne Vulgaris."
- International Journal of Women's Dermatology. "Management of Acne in Skin of Color."
This content is for informational purposes only and does not constitute medical advice. Consult a qualified healthcare professional for diagnosis and treatment.




