Non-Invasive Chickenpox Scars: A Guide to Post-Varicella Skin
Non-invasive chickenpox scar treatments range from microneedling to chemical peels and topical therapies. Discover which clinical interventions reduce varicella scarring without surgery.

What the Evidence Says About Non-Invasive Treatment for Chickenpox Scars
Non invasive chickenpox scars treatments are a well-established category of clinical interventions that can meaningfully reduce the appearance of varicella-zoster scarring without surgery. For those seeking a quick orientation, the most evidence-supported options are:
- TCA CROSS (chemical peeling) - the most studied method; 70% TCA showed >75% improvement in 41% of patients
- Microneedling - safe for all skin types including darker tones; typically 3-8 sessions
- Laser resurfacing (Er:YAG, CO2, Nd:YAG) - Er:YAG demonstrated average 55% improvement in a single session
- Microdermabrasion - gentle option with low side-effect profile; particularly useful for darker skin
- Topical agents (retinoids, rosehip seed oil) - modest evidence; best for pigmentation rather than deep atrophy
Chickenpox is far less common today than it was a generation ago — the vaccine has reduced infection rates by over 90%. But for anyone who contracted varicella-zoster virus before widespread immunization, the skin can carry a lasting record of the illness.
Research estimates that between 7 and 18% of post-varicella patients develop permanent depressed scars. Among those, approximately 40% of scars appear on the face — where they are most visible and most likely to affect confidence and social ease.
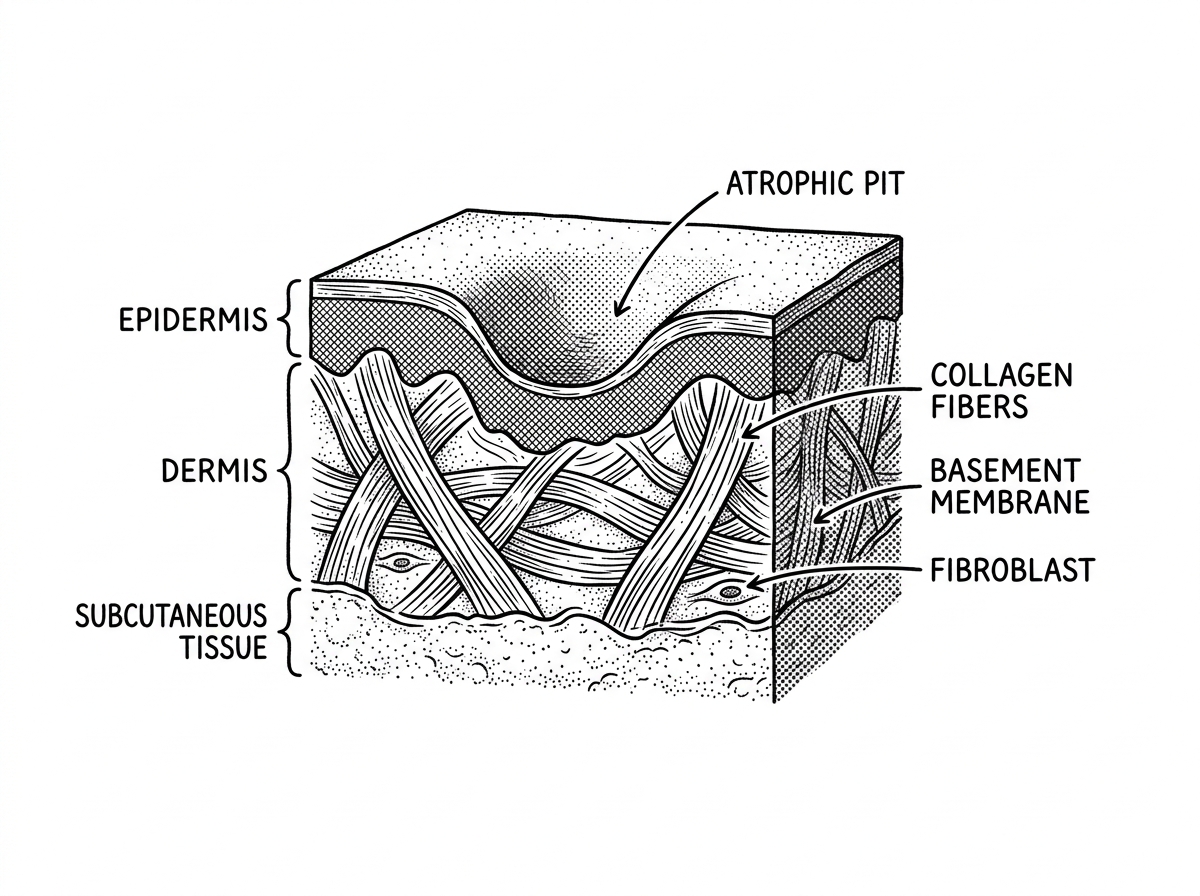
These scars form through a specific biological process. During active chickenpox, the varicella-zoster virus drives intense inflammation in the skin. When blisters are scratched or become secondarily infected, the damage extends into the dermis — the deeper structural layer of the skin. This disrupts normal collagen production and repair, leaving behind the characteristic round, sunken (atrophic) pits that many adults still carry decades later.
Unlike acne scars, which originate from deeper pilosebaceous units, chickenpox scars tend to involve the epidermal layer and present with a more uniform depressed morphology. This distinction matters clinically, because it influences which treatments are most likely to work.
The encouraging news: non-invasive and minimally invasive treatments have a growing evidence base — and several can produce significant, lasting improvement without surgery.
This content is for informational purposes only and does not constitute medical advice. Consult a qualified healthcare professional for diagnosis and treatment.
Pathogenesis and Classification of Varicella-Zoster Scarring
To understand how to treat a chickenpox scar, one must first understand the biological "wreckage" left behind by the virus. When the varicella-zoster virus infects the skin, it creates vesicles (blisters) that trigger a significant inflammatory response. Research indicates that this inflammation destroys collagen, the structural protein responsible for skin volume and elasticity.
The Biological Mechanism of Atrophy
When the skin attempts to heal after the viral infection, it may fail to regenerate enough collagen to fill the space where the vesicle was located. This results in an atrophic, or "pitted," scar. Unlike a typical cut that might leave a raised line, a chickenpox scar is a deficit of tissue. Prevalence studies show that about 1 in 5 people who have had chickenpox will develop at least one such permanent mark.
Classification of Chickenpox Scars
Clinical observation typically divides these scars into three primary categories:
- Atrophic Scars: The most common type. These appear as small, round, sunken "divots" or "pits." They are often 5–10mm in diameter.
- Hypertrophic Scars: Less common, these are raised, firm bumps that occur when the body produces too much collagen during repair.
- Pigmentary Changes: These are not structural scars but rather areas of post-inflammatory hyperpigmentation (dark spots) or hypopigmentation (white spots).
| Feature | Chickenpox Scars | Acne Scars |
|---|---|---|
| Origin | Viral infection (Epidermal/Dermal) | Bacterial/Hormonal (Pilosebaceous unit) |
| Shape | Uniformly round, "punched out" | Varied (icepick, boxcar, rolling) |
| Depth | Often involves the epidermal layer | Usually deeper into the dermis |
| Common Site | Face, trunk, and limbs | Primarily face, back, and chest |
Clinical Approaches to Non Invasive Chickenpox Scars
The primary goal of treating non invasive chickenpox scars is dermal remodeling. This involves stimulating fibroblasts—the cells responsible for "building" skin—to produce new collagen and elastin, effectively plumping the sunken area from the bottom up. For more detailed insights, readers can explore chickenpox scar treatment for adults.
Collagen Induction for Non Invasive Chickenpox Scars
One of the most effective non-surgical methods is percutaneous collagen induction, commonly known as microneedling. This procedure involves using fine needles to create thousands of microscopic "micro-injuries" in the scar tissue.
Research suggests that this process can boost collagen production by up to 400%. Because it does not use heat (like some lasers), it is exceptionally safe for all skin types, including darker skin tones (Fitzpatrick IV-VI). A small report found that three monthly microneedling sessions significantly minimized discoloration and texture issues in a dark-skinned teenager. For a deeper look at this technology, see our guide on microneedling for scar reduction and atrophic scar microneedling therapy.
Subcision and Mechanical Release
Sometimes, the reason a chickenpox scar remains sunken is that fibrous bands of scar tissue are physically "tethering" the skin to the underlying layers. Subcision is a minimally invasive technique where a dermatologist uses a small needle to sweep under the scar and break these bands.
A study on the subcision-suction method found that following the procedure with regular suctioning (using a specialized device) helped prevent the skin from re-tethering, resulting in a 71% mean improvement in scar appearance.
Comparative Analysis of Energy-Based and Chemical Treatments
When topical creams aren't enough, energy-based devices and chemical reconstruction offer higher-tier results. These treatments are often categorized by how they interact with the skin surface.
Laser Resurfacing for Non Invasive Chickenpox Scars
Lasers use targeted light energy to either remove thin layers of skin (ablative) or stimulate deeper layers without damaging the surface (non-ablative).
- Er:YAG Laser: This is highly effective for "pitted" scars. One study showed an average 55% improvement in chickenpox scars after just a single session.
- Pico Lasers: These are ultra-fast lasers that address both pigmentation and early collagen loss with minimal downtime.
- Fractional CO2: Often considered the "gold standard" for severe texture issues, though it requires more recovery time than non-ablative options.
For a comprehensive comparison of these technologies, see our laser treatment for scars complete guide.
Chemical Reconstruction of Skin Scars (CROSS)
The TCA CROSS technique is perhaps the most specific non-invasive treatment for "punched-out" chickenpox scars. It involves applying a high concentration of trichloroacetic acid (TCA) directly into the base of the scar using a toothpick or fine applicator.
This causes a localized "frosting" and controlled inflammation that triggers the formation of new collagen. A 2012 study of 100 patients using 70% TCA CROSS found that 41% of participants saw "marked improvement" (>75%), while another 42% saw "moderate improvement."
The Role of Topical Agents and Prevention Strategies
While clinical procedures offer the most dramatic results, topical agents play a vital role in preparing the skin and managing minor scars.
Evidence-Based Topicals
- Retinoids: Derivatives of Vitamin A, such as tretinoin, are clinically proven to boost collagen. Research suggests using 0.05% tretinoin cream nightly for 2 to 4 weeks before laser treatments can actually improve the outcome.
- Rosehip Seed Oil: This oil is rich in vitamins and antioxidants. A small study found that rosehip oil applied twice daily for 12 weeks significantly improved redness and discoloration on surgical scars, suggesting potential benefits for recent chickenpox marks.
- Silicone Sheets: While most effective for raised scars, silicone can help maintain hydration and normalize the healing environment for newer atrophic scars.
Prevention During Active Infection
The best way to treat a scar is to prevent it from forming. During an active varicella-zoster infection, the following steps are recommended:
- Early Antivirals: Taking medications like Acyclovir or Valacyclovir within 24 hours of the rash appearing can lower the total lesion count and reduce inflammation.
- Mitigate Scratching: Scratching is the primary cause of secondary infection and deeper dermal damage. Use antihistamines, oatmeal baths, and calamine lotion to manage itch.
- Wound Care: Proper wound care is essential. Keeping the blisters moist with plain petroleum jelly and covered can prevent the hard scabs that often lead to deeper pits.
Conclusion
The "ghosts" of chickenpox past no longer have to be permanent fixtures on the skin. From the focal precision of TCA CROSS to the broad-spectrum remodeling of microneedling and lasers, modern dermatology offers several paths to smoother skin.
A typical treatment timeline involves 3 to 6 sessions spaced 4 to 6 weeks apart. While results are not instantaneous—collagen remodeling takes months—the improvements are generally permanent once achieved. It is always advisable to consult a board-certified dermatologist to determine which specific combination of non invasive chickenpox scars treatments is right for your skin type and scar depth.
Frequently Asked Questions
Are non-invasive treatments effective for old chickenpox scars? Yes. While newer scars respond more quickly, even decades-old scars can be significantly improved through microneedling, subcision, and laser resurfacing, as these treatments "re-start" the body's natural healing response.
How many sessions are typically required for visible results? Most patients require 3 to 8 sessions to see significant improvement. Minor pigmentation may fade in 2 to 3 sessions, while deep atrophic pits usually require more intensive remodeling over 6 months.
Can non-invasive treatments be used on darker skin tones? Absolutely. However, care must be taken with certain lasers. Microneedling and TCA CROSS are often preferred for Fitzpatrick IV-VI skin types because they carry a lower risk of post-inflammatory hyperpigmentation compared to aggressive ablative lasers.
Works Cited
- Agarwal, N., et al. (2013). Chemical reconstruction of skin scars therapy using 100% trichloroacetic Acid in the treatment of atrophic facial post varicella scars: a pilot study. Journal of Cutaneous and Aesthetic Surgery.
- Barikbin, B., et al. (2012). Focal high-concentration trichloroacetic acid peeling for treatment of atrophic facial chickenpox scar: An open-label study. Dermatologic Surgery.
- Kye, Y. C. (1997). Resurfacing of pitted facial scars with a pulsed Er:YAG laser. Dermatologic Surgery.
- Leung, A. K., et al. (2001). Scarring resulting from chickenpox. Pediatric Dermatology.
- Valerón-Almazán, P., et al. (2015). Evolution of post-surgical scars treated with pure rosehip seed oil. Journal of Cosmetics, Dermatological Sciences and Applications.
This content is for informational purposes only and does not constitute medical advice. Consult a qualified healthcare professional for diagnosis and treatment.




