The Science of Softening Your Scars
Scar tissue massage therapy uses targeted pressure and movement to improve flexibility and appearance. Discover the science behind this hands-on technique and how to do it effectively.

What Is Scar Tissue Massage Therapy — and Does It Work?
Scar tissue massage therapy is a hands-on technique that uses targeted pressure and movement to improve the flexibility, appearance, and function of scar tissue after surgery or injury.
Here is what the evidence currently shows:
| Question | Short Answer |
|---|---|
| When to start | Once the wound is fully closed — typically 2-3 weeks post-surgery |
| How often | 2-3 times daily, 5-10 minutes per session |
| How long | Continue for 6 months to 1 year |
| Key benefit | Prevents adhesions, improves mobility, reduces pain and itching |
| Main techniques | Circular, linear, and cross-friction strokes |
| When to stop | During active radiation therapy or if skin is open or inflamed |
Scars are not simply cosmetic. Beneath the surface, scar tissue is structurally different from healthy skin — it is less elastic, less well-supplied with blood, and prone to sticking to underlying layers of muscle and fascia. This can cause tightness, restricted movement, and ongoing discomfort long after the original wound has healed.
For many people — particularly those recovering from breast cancer surgery, orthopedic procedures, or significant skin injuries — these physical restrictions become a real quality-of-life issue.
The encouraging reality is that scar tissue is living tissue. It continues to remodel itself for months, sometimes years, after injury. Research suggests that targeted massage may support this remodeling process by improving collagen alignment, increasing local circulation, and reducing the formation of adhesions.
A 2023 review examining seven clinical trials and 420 burn patients found that scar massage was associated with measurable reductions in pain, scar thickness, itching, and anxiety — though the authors noted that study designs varied and further research is needed to establish optimal protocols.
This article explains the biology behind scar formation, reviews the current evidence for massage therapy as a management tool, and provides practical, science-informed guidance on technique, timing, and safety.
This content is for informational purposes only and does not constitute medical advice. Consult a qualified healthcare professional for diagnosis and treatment.
Key terms for scar tissue massage therapy:
The Biological Mechanism of Scar Formation
To understand why scar tissue massage therapy is effective, one must first understand how the body repairs itself. When the dermis (the deep layer of the skin) is damaged, the body initiates a rapid repair mission. This process is less about "regeneration" and more about "patching."
Healthy skin is composed of collagen fibers arranged in a flexible, "basket-weave" pattern. This structure allows the skin to stretch in multiple directions. However, during the proliferative phase of wound healing, the body produces collagen in a hurried, haphazard fashion. According to a literature review on wound healing, these new fibers often align in a single, parallel direction.
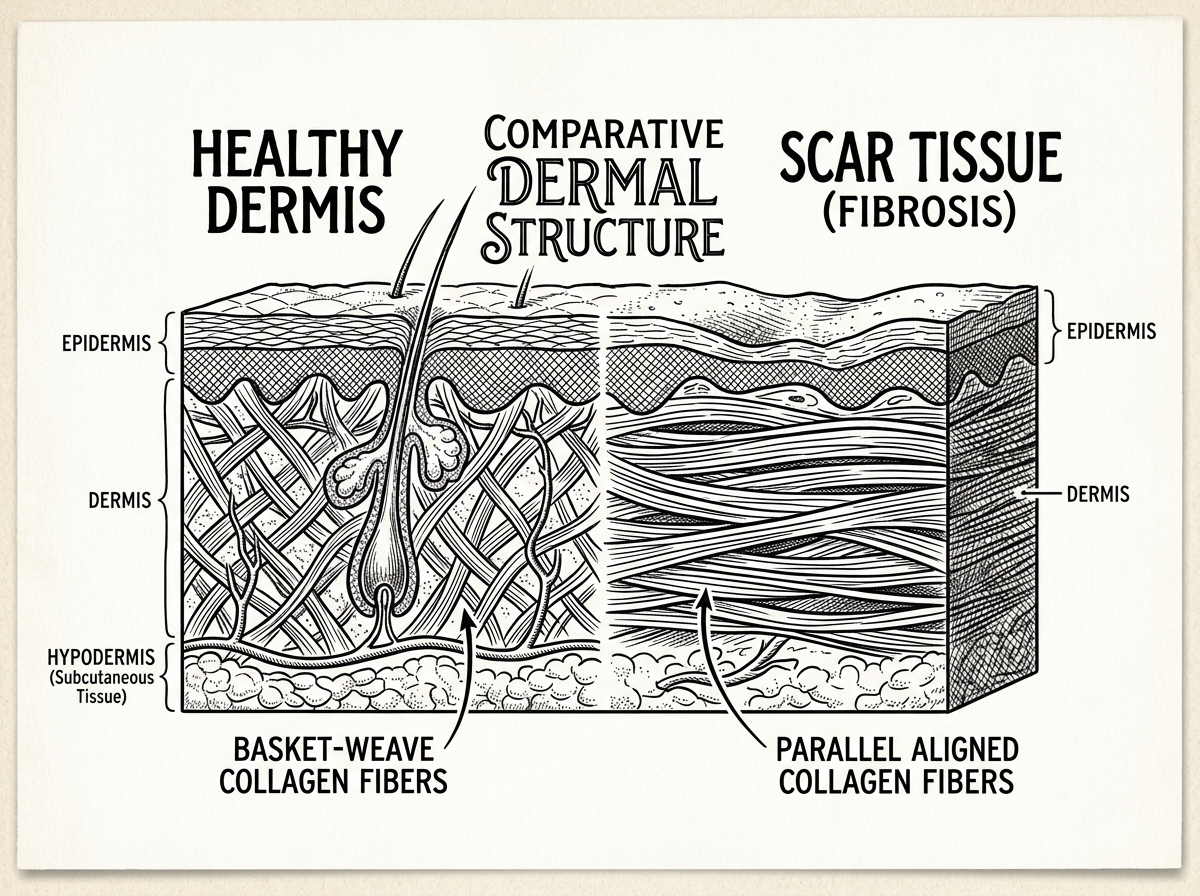
This parallel alignment results in tissue that is structurally inferior to the original skin. It lacks hair follicles and sweat glands, and its tensile strength typically only reaches 70-80% of normal skin. Because these fibers are densely packed and lack elasticity, they can form "adhesions"—internal bonds where the scar "sticks" to underlying muscles, tendons, or fascia. This biological reality is the primary reason why more info about scar healing is essential for those experiencing post-surgical tightness.
The Role of Scar Tissue Massage Therapy in Recovery
The application of mechanical force to a scar is not just about comfort; it involves a biological process called mechanotransduction. This is the way cells convert mechanical stimuli (like the pressure from a thumb) into chemical signals. When a therapist or patient applies pressure, it signals the fibroblasts—the cells responsible for collagen production—to remodel the tissue.
Research indicates that scar tissue massage therapy helps prevent tissue hypoxia (lack of oxygen) by stimulating microcirculation. A systematic review and meta-analysis on burn scars suggests that regular mobilization can significantly improve the pliability of the tissue. By physically moving the skin over the underlying structures, the massage "breaks" the small cross-links of collagen that cause adhesions, allowing the different layers of tissue to slide and glide against each other once more.
Evidence-Based Benefits of Scar Tissue Massage Therapy
Clinical observations and peer-reviewed studies highlight several key benefits of consistent scar mobilization:
- Improved Pliability: Massage helps soften the "hard" feeling of a scar, making it more flexible and less prone to cracking or reopening.
- Pruritus (Itching) Reduction: By modulating the nerve endings in the area and improving hydration, massage can decrease the intense itching often associated with maturing scars.
- Increased Range of Motion: Mobilizing scars that cross joints (like the knee or shoulder) prevents the tissue from shortening and restricting movement.
- Pain Desensitization: New scars are often hypersensitive. Gentle, repetitive touch helps the nervous system habituate to sensation, reducing pain over time.
- Collagen Realignment: Mechanical pressure encourages collagen fibers to move from a random, tangled state into a more organized, functional alignment.
Implementing Scar Tissue Massage Therapy at Home
While professional therapy is highly beneficial, much of the work in scar remodeling happens through consistent daily self-care. Professionals generally recommend the following guidelines for home-based care:
- The Blanching Test: Apply enough pressure so that the skin under your finger turns white (blanches) and then turns pink again when you let go. This ensures you are reaching the deeper layers of tissue, not just sliding over the surface.
- Duration and Frequency: Aim for 5 to 10 minutes per session, performed 2 to 3 times a day.
- Consistency: The remodeling phase of a scar can last up to two years. For the best results, this routine should be maintained for at least the first six months.
- Warmth: Massage is often more effective when the skin is warm, such as after a shower, as the heat increases tissue extensibility.
For those looking to deepen their understanding of long-term care, seeking more info about scar healing can provide additional strategies for managing complex scars.
Clinical Techniques for Manual Scar Remodeling
Professional massage therapists and physical therapists utilize specific strokes designed to target different aspects of the scar's structure.
- Cross-Friction (Transverse Friction): This involves moving the finger pads perpendicular to the line of the scar. This technique is specifically designed to prevent or break down adhesions between the scar and the underlying muscle or bone.
- Circular Mobilization: Using the pads of the fingers, the therapist makes small, firm circles over the entire length of the scar and the surrounding skin. This helps "loosen" the tissue in all directions.
- Linear Strokes: These are firm strokes moving along the length of the scar. This helps to lengthen the tissue, which is particularly important for scars that feel "tight" or "short."
- Myofascial Release: This involves applying a gentle, sustained stretch to the skin adjacent to the scar to restore the "slide and glide" of the fascial layers.
- Trigger Pointing and Acupressure: In some cases, therapists apply sustained pressure to specific "knots" or sensitive points within the scar. This can induce an ischemic reaction—where blood is briefly pushed out and then floods back in—which helps soften the tissue.
Research into instrument-assisted soft tissue mobilization (IASTM) shows that using specialized tools can also be effective, though manual therapy remains the gold standard for patient comfort and feedback.
Specialized Approaches for Surgical Recovery
Different surgeries require tailored approaches to scar tissue massage therapy:
- Breast Cancer Surgery: Massage is vital for scars on the chest and armpit to prevent "cording" (axillary web syndrome) and to maintain shoulder mobility.
- Kidney Transplant: Abdominal scars can affect core strength and even breathing if they become too restrictive. Massage helps maintain the flexibility of the abdominal wall.
- C-Section: Deep massage can help prevent the scar from adhering to the bladder or uterus, which can sometimes cause pelvic discomfort.
- Orthopedic Incisions: For knee or hip replacements, massage ensures the scar doesn't "tether" the joint, which would limit the success of the replacement.
Safety Protocols and Clinical Contraindications
Safety is paramount when working with healing tissue. Massaging a wound too early can lead to infection or cause the wound to reopen (dehiscence).
The "Ready" Signals: Before beginning scar tissue massage therapy, ensure the wound is fully epidermized. This means there are no open areas, no oozing, no scabs, and all stitches or staples have been removed. This usually occurs 2 to 3 weeks after the initial injury or surgery.
When to Avoid Massage:
- Infection: If the area is hot, excessively red, swollen, or draining fluid, stop immediately and consult a doctor.
- Radiation Therapy: Skin that is currently undergoing radiation is extremely fragile. Massage should be paused during treatment and only resumed once the skin has fully recovered, as advised by an oncologist.
- Inflammatory Stage: During the very first few days of healing, the tissue is too weak for deep pressure.
- Fragile Epidermis: If the skin is paper-thin or prone to blistering, only the gentlest touch should be used.
For those prone to keloids and hypertrophic scars, professional guidance is essential, as aggressive massage can sometimes trigger further collagen overproduction in these specific scar types.
Frequently Asked Questions about Scar Management
When is it safe to begin scar massage after surgery?
The general clinical consensus is to wait until the wound is completely closed. This typically means all scabs have fallen off naturally and any sutures or staples have been removed. For most surgical patients, this window opens between 14 and 21 days post-operation. Always obtain clearance from your surgeon before starting.
Can massage therapy improve the appearance of mature scars?
The "maturation phase" of a scar lasts between 12 and 24 months. During this window, the tissue is still actively remodeling and is quite responsive to massage. Once a scar is "mature" (usually white, flat, and older than two years), it is less likely to change significantly in appearance. However, massage can still help improve the flexibility of the surrounding skin and reduce any lingering tightness.
What lubricants are recommended for scar mobilization?
In the clinical setting, some therapists prefer "dry" techniques to ensure they have a firm grip on the tissue, allowing them to move the scar rather than just sliding over the skin. However, for home use, lubrication can prevent irritation.
- Recommended: Fragrance-free moisturizers, plant oils (like jojoba or almond oil), or silicone-based gels.
- Avoid: Heavily perfumed lotions or products with "miracle" claims that haven't been peer-reviewed.
Conclusion
The journey of healing does not end when the stitches come out. Scar tissue is a dynamic, living part of the body that requires ongoing care to reach its most functional state. By understanding the science of scar tissue massage therapy, patients can take an active role in their recovery, moving from a state of restriction to one of mobility.
While the physical changes—a flatter, softer, or paler scar—are often the most sought-after, the improvements in quality of life are the most significant. Reducing pain, regaining the ability to reach into a cupboard, or simply feeling "at home" in one's skin again are the true goals of scar management. For continued education and resources, visiting more info about scar healing can empower patients with the latest evidence-based strategies.
This content is for informational purposes only and does not constitute medical advice. Consult a qualified healthcare professional for diagnosis and treatment.




